Down syndrome in pregnancy: A new chapter in your family’s story
January 13, 2026

Every pregnancy has its own story. For some families, that story includes a moment when a screening exam or ultrasound finding raises the possibility of Down syndrome. That moment can bring a swirl of emotions, including helplessness in knowing where to go for more information, concern about how the diagnosis may impact pregnancy or delivery, and overall uncertainty about the future.
As a maternal-fetal medicine specialist, I’ve walked alongside many families during this chapter, and I’ve seen how information, preparation, and community can turn that uncertainty into confidence.
Down syndrome is just one part of a child’s story, and understanding what it means during pregnancy is the first step in supporting their unique path.
What is Down syndrome?
Human cells generally have 46 chromosomes. A special type of cell division called meiosis creates the mother’s egg cell and the father’s sperm cell, each with only 23 chromosomes. Those cells join during fertilization, resulting in 46 chromosomes.
But sometimes a random error in that cell division includes an extra copy of the 21st chromosome. The error occurs more often with egg cells, but it can also occur in sperm cells. The embryo thus ends up with three copies of the 21st chromosome instead of the usual two. This is known scientifically as trisomy 21, but it is more commonly known as Down syndrome.
Down syndrome is one of the most common genetic disorders. Each year, about 5,700 babies, or one in every 640, are born with Down syndrome in the U.S.
Down syndrome can occur in any pregnancy. Most cases are spontaneous – no behavior, diet, or exposure causes or prevents it. However, a few factors can increase the odds:
- Maternal age: The chances of having a baby with Down syndrome gradually rise as a woman’s egg cells age. The delineation for “advanced maternal age” historically has been 35, though that number is more of a guideline than a strict threshold.
- Previous pregnancy with a chromosomal condition: Future pregnancies have slightly higher odds of resulting in a child with Down syndrome.
- Being a carrier of the genetic translocation for Down syndrome: This is when a piece of one chromosome breaks off and attaches to another, or when pieces from two chromosomes swap places. Either parent can pass on the genetic translocation for Down syndrome.

A brief history of Down syndrome
John Langdon Down is credited with the discovery of the disorder now known as Down syndrome. The English physician was a medical superintendent at an asylum in the mid-1800s and noticed that many patients had similar physical features. His published work in 1866 fully classified the condition for the first time.
By the early 1900s, doctors realized that children with these features were more likely to be born to women later in their child-bearing years. Advancements in the 1950s allowed researchers to count the exact number of chromosomes inside human cells for the first time.
The first prenatal diagnosis of Down syndrome was made in the late 1960s, and by the late 1970s, the National Institutes of Health announced that all pregnant women age 35 and older should be offered a test, an amniocentesis, to diagnose chromosome abnormalities.
It wasn’t until the 1980s that a non-invasive screening test was developed using a maternal blood sample. Since then, further advancements to screening methods have produced higher detection rates.
What screenings can point to Down syndrome?
There are generally two reasons that Down syndrome initially is brought up during pregnancy: screening test results and “soft markers” (physical findings) discovered during an ultrasound.
Noninvasive prenatal testing
The American College of Obstetricians and Gynecologists (ACOG) recommends that patients are offered noninvasive prenatal testing (NIPT) during every pregnancy to give them and their pregnancy care team more information. NIPT is a screening test and does not diagnose a condition. It only tells us whether there is a higher or lower chance for a condition such as Down syndrome.
This simple blood test, which is available as early as 10 weeks, looks at fetal DNA in the mother’s blood. It is the most accurate screening tool for Down syndrome available today, and it has very good sensitivity and specificity. A low-risk result is reassuring but not a guarantee; a high-risk result does not confirm a diagnosis but signals the need for a conversation about diagnostic testing.
Soft markers found during an ultrasound
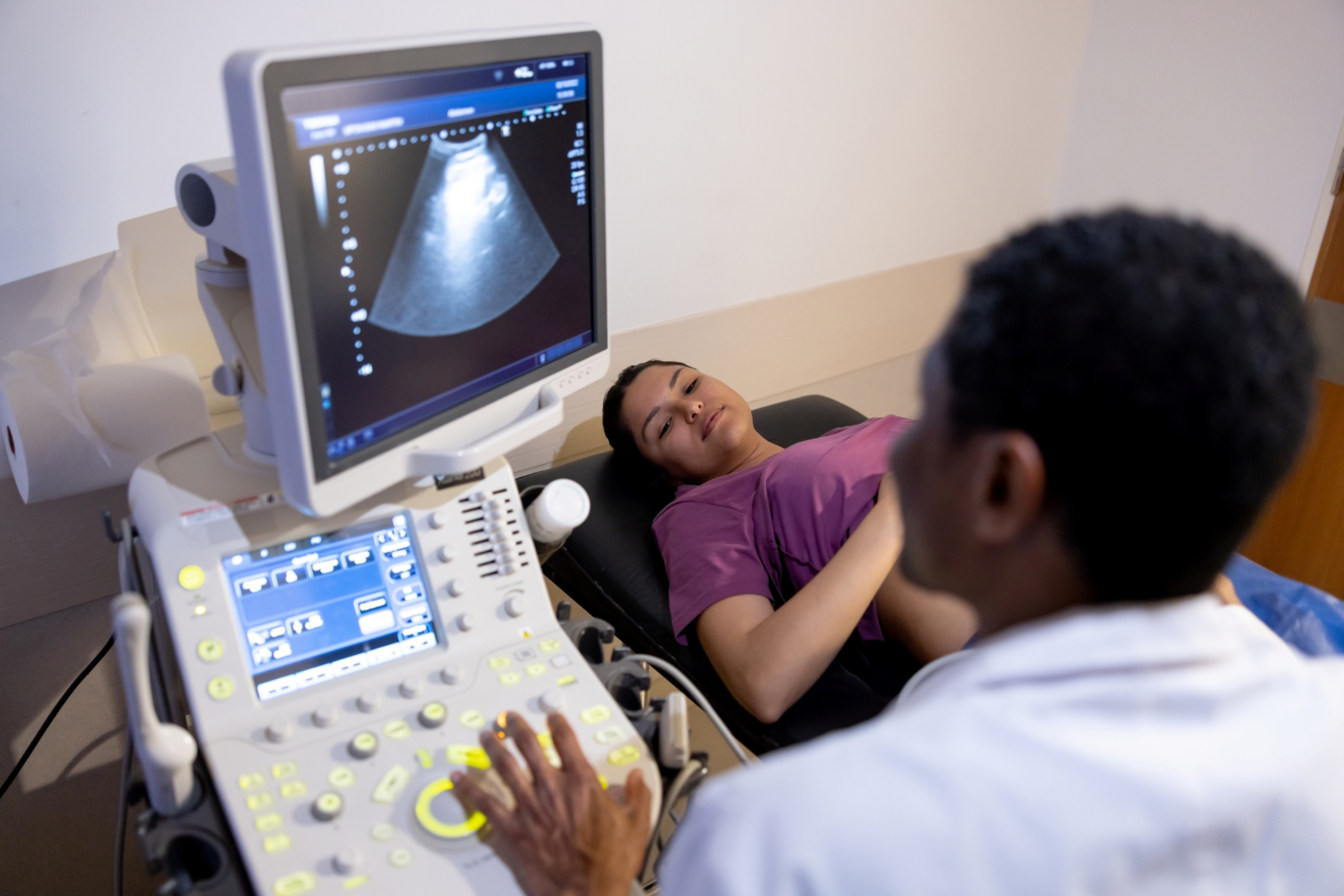
Soft markers are features seen during an ultrasound that may indicate an increased likelihood of a chromosomal abnormality. A soft marker is not a malformation or birth defect; some of the features can also appear in a typical pregnancy.
Some soft markers for Down syndrome include:
- Small or absent nasal bone seen in either the ultrasound taken during the first trimester (11-14 weeks) or on the later anatomy ultrasound
- Increased thickness of the nuchal translucency (11-14 weeks)
- Increased thickness of the nuchal fold, a fluid filled space located at the back of the neck (16-20 weeks)
- Enlarged brain ventricles
- Small, bright spot on the heart (echogenic intracardiac focus, or EIF)
- Abnormal aortic arch of the heart (aberrant right subclavian artery, or ARSA)
- Bowel that appears whiter on ultrasound (echogenic bowel)
- Mild kidney swelling (dilation of the renal pelvis)
- Shorter upper arm or thigh bones
Some soft makers have a stronger association with Down syndrome than others. For example, EIF occurs in as many as 5% of pregnancies and is even more common in babies with Asian ethnicity, while an enlarged nuchal fold or absent nasal bone is not commonly seen and yields a higher association with Down syndrome.
If we see soft markers in your ultrasound, we will review them with you in the context of your screening results, medical history, and what matters most to you in terms of information and level of certainty.
How can you find out for sure?
If you get a screening result or ultrasound finding that raises concern, you may consider diagnostic testing to analyze a sample of the fetal chromosomes.
These can include:
- Chorionic villus sampling (CVS): Typically performed between 11 and 13 weeks of pregnancy by taking a sample from the placenta.
- Amniocentesis: Can be done after week 16 of pregnancy by collecting fetal cells from the amniotic fluid around the baby.
Despite what you might have heard, amniocentesis and CVS have a less than 0.2% risk of miscarriage. UT Southwestern maternal-fetal medicine specialists follow the most advanced protocols to reduce the risk of procedure-associated complications.
Diagnostic testing for Down syndrome is optional. Some parents want to know ahead of time so they can have certainty. Others choose not to pursue further testing and may prefer to defer diagnostic testing until after birth. The best choice is the one that feels right for you, and we will be by your side with information and support as you make your decision.
Expect an ordinary pregnancy and delivery
Most pregnancies with Down syndrome progress normally, and your care likely will be managed in much the same way as any other pregnancy. That said, we do watch a few things more closely as the baby grows:
- Detailed anatomy ultrasound: All pregnancies typically get an ultrasound at around 20 weeks, but if there is an increased risk, you should have a higher-level ultrasound called a detailed fetal anatomic survey. We examine the entire baby, including the heart, kidneys, stomach, brain, limbs, and spine to assess growth and development. While some babies with Down syndrome have minimal structural differences, heart defects are more common, so careful assessment is essential.
- Fetal echocardiogram: About half of babies born with Down syndrome have a heart defect, so if there is increased concern, a fetal echo will be offered. This specialized ultrasound takes precise measurements of the fetal heart valves and blood flow. Even if the anatomy scan appears normal, a fetal echo can spot small differences.
- Growth monitoring: Because the placenta also carries an extra chromosome, there can be a risk for growth restriction or changes in placental function. We’ll closely track the baby’s growth throughout the pregnancy.
- Monitoring for rare complications: A very small number of babies with Down syndrome may develop conditions such as hydrops (excessive fluid in the tissues or organs) or transient leukemia, and there is an increased risk for stillbirth. While these conditions are rare, your care team will keep a close eye on fluid levels, movement patterns, and blood flow.
Delivery is usually no different from a typical pregnancy. Both delivery timing and type of delivery – vaginal or cesarean (C-section) – are based on other factors in the pregnancy and typical obstetric indications.
The baby’s overall health in pregnancy may influence where you plan to deliver. For example, you may wish to choose a hospital with a neonatal intensive care unit or a pediatric heart specialist on staff. While many babies with Down syndrome do not need additional care at birth, there are some tests specific to Down syndrome babies and you’ll want to choose a center that can offer you those.
Pediatrics; Your Pregnancy Matters
6 things to expect with babies with Down syndrome
- Jessica Morse, M.D.
April 25, 2025
The next chapters of your family’s story
Newborns with Down syndrome often grow well and thrive with a little extra support in the beginning. These babies often need:
- Feeding support: Lower muscle tone can make early feeding more challenging. We’ll make sure you have support and follow-up from lactation consultants and feeding specialists.
- Developmental monitoring: Babies with Down syndrome grow along their own expected curve. Your pediatrician will use specific growth charts designed to show your child’s progress.
- Screening tests after birth: Pediatric teams often check thyroid function, heart structure, and newborn blood count and watch for possible vision or hearing issues.
- Motor skill development: Because muscle tone may be lower, physical or occupational therapy can support milestones such as sitting, crawling, and walking.
- Academic support: Almost all people with Down syndrome have a mild to moderate learning disability. Pediatric specialists can help identify the support services your child may need to succeed in school.

While the early years may involve extra therapy visits and the school years bring the need for advocacy in the educational system, many children with Down syndrome grow up to become extraordinary adults who pursue regular work, have meaningful friendships and possibly romantic relationships, and enjoy clubs and hobbies alongside their peers.
Due to shifts in the societal mindset of what is possible along with access to services, people with Down syndrome are now achieving previously unanticipated goals such as completing triathlons, earning a college degree, or becoming a business owner, actor, model, or motivational speaker.
With advances in access to cardiology, other medical care, and adult Down syndrome care, the life expectancy for those with Down syndrome has increased dramatically over the last 40 years. People who have Down syndrome have not changed in capability or health over the years; instead, society has improved support to allow them to fulfill their potential. With the right support, the possibilities are endless.
Fill your world with exceptional characters
Connection matters. Parents often tell me that meeting other families on a similar journey was one of the most important steps they took. Talk with your doctor about local Down syndrome organizations, such as children’s playgroups and family education programs, as well as recommendations for early childhood specialists to help your baby thrive.
National organizations can help connect expectant parents with trained volunteer families raising a child with Down syndrome, often in your local area. These families can offer real-life perspective, encouragement, and practical tips.
Having a baby with Down syndrome is just a different version of the story you imagined. Studies show siblings of those with Down syndrome often have enhanced empathy and compassion as well as predominantly positive psychosocial outcomes with over 96% reporting affection toward their sibling.
Receiving unexpected news during pregnancy can stir a range of emotions. And one I see most often from my patients is curiosity: What do I need to know to make the right decisions for my family? Your health care team will walk with you through this process to support and celebrate your family every step of the way.
To talk with an expert about pregnancy and Down syndrome, make an appointment by calling 214-645-3838 or request an appointment online.












