First dual HIV-positive organ transplant in Texas gives Dallas man HOPE
November 11, 2020

For many years, HIV-positive patients diagnosed with liver or kidney failure faced a long wait and fewer options for organ transplantation than patients without HIV.
But today, those patients have new HOPE.
The HIV Organ Policy Equity (HOPE) Act of 2013 makes it possible for someone with HIV to donate their organs, and under the direction of a large clinical trial sponsored by the National Institutes of Health (NIH), those organs will be matched to an HIV-positive recipient.
UT Southwestern’s transplant program is a site that participates in this groundbreaking research, and this summer our team of doctors, surgeons, and infectious disease specialists helped a 53-year-old Dallas man become the first recipient of an HIV-positive to HIV-positive organ transplant in Texas. Here is his story.
‘It’s rejuvenating’
Within three weeks of being placed on an organ transplant list for HIV-positive patients this spring, John Welch got the call. A liver was available from a deceased donor, and it was an excellent match.
The previous four years had not moved so quickly for Mr. Welch.
In 2016, he was diagnosed with HIV and cirrhosis of the liver on the same day. (People with HIV are at an increased risk of developing end-stage kidney and liver disease.)
Later that year, he was admitted to Parkland Memorial Hospital with a near-fatal case of pneumonia and he lost 90 pounds. While he was being treated, he noticed that many of the doctors caring for him wore ID badges that identified them as UT Southwestern faculty.
“They saved my life,” he said. “They absolutely saved my life.”
Mr. Welch said he quit drinking alcohol and started taking antiviral medication to keep the HIV at bay, but over the next several years his health deteriorated. By the time he got the transplant call, he was in the early stages of liver failure, suffering from mild confusion and memory loss.
“I want to do something with purpose, and raise awareness that HIV-positive people can be organ donors. I am a walking testament to that.”
John WelchFirst recipient of an HIV-positive to HIV-positive organ transplant in Texas
If it wasn’t for the HOPE Act and UT Southwestern’s participation in the NIH clinical trial, he said he probably would have had to wait much longer for a donor.
“I had the utmost confidence in the team at UT Southwestern. I never had better treatment,” Mr. Welch said. “Everyone there is genuinely concerned and really cares about the patient.”
On July 1, UT Southwestern’s liver transplant team, led by Dr. Steven Hanish, Medical Director of Liver Transplantation, along with Parsia Vagefi, Chief of the Division of Surgical Transplantation, completed Mr. Welch’s liver surgery without complications at William P. Clements Jr. University Hospital.
By September, he was recovering at home, back to playing piano and making plans for the future.
“The organ I got was from a young man, and I think it’s rejuvenating this old, tired bag of bones,” Mr. Welch says with a smile. “Maybe I’ll be 25 again!”
Expanding the transplant pool
As an academic medical center, UT Southwestern considers it part of our mission to pursue life-saving treatments for our patients.
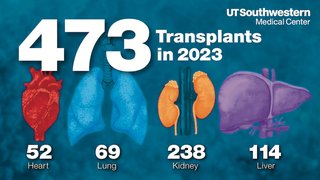
In 2019, our liver transplant program recorded the highest volumes of any in North Texas while maintaining one of the shortest lengths of stay for post-transplant patients in the country. Our kidney and lung transplant program are similarly delivering large volumes and excellent long-term survival rates.

So, when the HOPE Act expanded the organ donor pool, we took the necessary steps to become enrolled as an approved site for the NIH clinical trial because we knew it would help us offer treatment options to patients who didn’t have many before.
Our multidisciplinary approach to Mr. Welch’s transplant meant that UT Southwestern infectious disease specialist Ricardo La Hoz, M.D., would tend to his HIV status throughout the process.
“We use all the information that we have available on the donor and the recipient to design an HIV therapy that will cover both,” Dr. La Hoz said, explaining that his team will continue to monitor the patient’s test results to make sure that his HIV infection stays controlled. If it does not, his antivirals will be adjusted.
To date, Dr. La Hoz added, no patient who has received an organ transplant under the HOPE Act nationwide has developed uncontrolled HIV infection, known as HIV virologic failure.
As he follows up with his team of doctors at UT Southwestern, Mr. Welch said they are taking every precaution to keep him safe from exposure to COVID-19. He is looking forward to returning to his supportive circle of friends after the pandemic, but for now he is content to embrace life and share his story of hope.
“I want to do something with purpose, and raise awareness that HIV-positive people can be organ donors,” he said. “I am a walking testament to that.”