For centuries, gout was famously branded as the "disease of kings" – a painful price paid for a life of excess and indulgence. Historical figures from Henry VIII to Benjamin Franklin have been depicted as tending to swollen, bandaged feet after nights of rich food and heavy drinking.
Today, we know that gout is not a condition reserved for royalty.
This complex form of inflammatory arthritis is a rapidly growing public health concern in the U.S. A national health survey estimated that 9.2 million adults (about 3.9% of the population) live with gout, and diagnoses are climbing as the population grows and ages.
Scientific advances over the past century have transformed gout from a poorly understood affliction into a well-characterized inflammatory disease. We know that gout is far more complex than diet alone. Age, genetics, kidney function, and medications all play a role in a person’s risk of developing gout.
UT Southwestern rheumatology experts are working to shift the narrative. While diet still matters, gout is often a hereditary metabolic condition that requires specialized medical care. We have effective treatments that can prevent painful flares, protect joints, and stop long-term complications.
What causes gout?
Gout is a type of chronic inflammatory arthritis caused by the buildup of uric acid in the blood, a condition known as hyperuricemia. Uric acid forms when the body breaks down purines, which are substances found naturally in the body and in certain foods.
Most mammals have an enzyme called uricase that further breaks down uric acid. Humans don’t, which allows uric acid to enter the bloodstream.
Under normal circumstances, uric acid dissolves in the blood and is filtered out through the kidneys. If uric acid levels become too high, it can form needle-like crystals that accumulate in a joint, triggering the body’s immune response. Gout often develops in the big toe, but it can also appear in the ankles, knees, wrists, elbows, and fingers.

Diet contributes only a small amount of our uric acid load. We now view gout as a complex metabolic condition influenced by:
- Genetics: Between 40% to 50% of people diagnosed with gout have a family history of the disease. Large genome-wide studies have identified specific genetic alleles that control uric acid transport genes. This explains why many patients report a family history of gout — and why lifestyle changes alone may not be enough.
- Kidney health: Because the kidneys are responsible for filtering out uric acid, chronic kidney disease is one of the biggest risk factors for developing gout. The reverse also holds true.
- Gender biology: Overall, men are diagnosed with gout more often than women. This is partly because estrogen acts as a natural agent that helps the kidneys excrete uric acid. A woman’s risk of gout increases after menopause when estrogen levels drop.
Research has also clarified the connection between gout and other health conditions. Gout commonly coexists with cardiovascular disease, hypertension, obesity, and diabetes. Managing gout effectively often means addressing these interconnected conditions as part of a comprehensive care plan.
What are the symptoms of gout?
Unlike other forms of arthritis, the hallmark signs of gout can come on suddenly, sometimes overnight. This is known as a “flare,” and symptoms can include:
- Severe joint pain: It may be so tender that even the pressure of a bed sheet or a sock is unbearable.
- Rapid swelling and redness: The joint becomes hot, red, and visibly inflamed.
- Systemic symptoms: Some patients may experience fevers, chills, and general malaise.
Untreated gout can lead to "intercritical" periods in which crystals continue to build up unnoticed. This eventually causes permanent joint erosions or the formation of tophi – large, chalky deposits of crystals that become infected, painful, or disfigured.
How is gout diagnosed?
Gout is highly treatable, but it requires an accurate diagnosis and a proactive approach to prevent long-term damage. A single gout flare can be intensely painful and is often a warning sign of underlying metabolic and kidney-related issues.
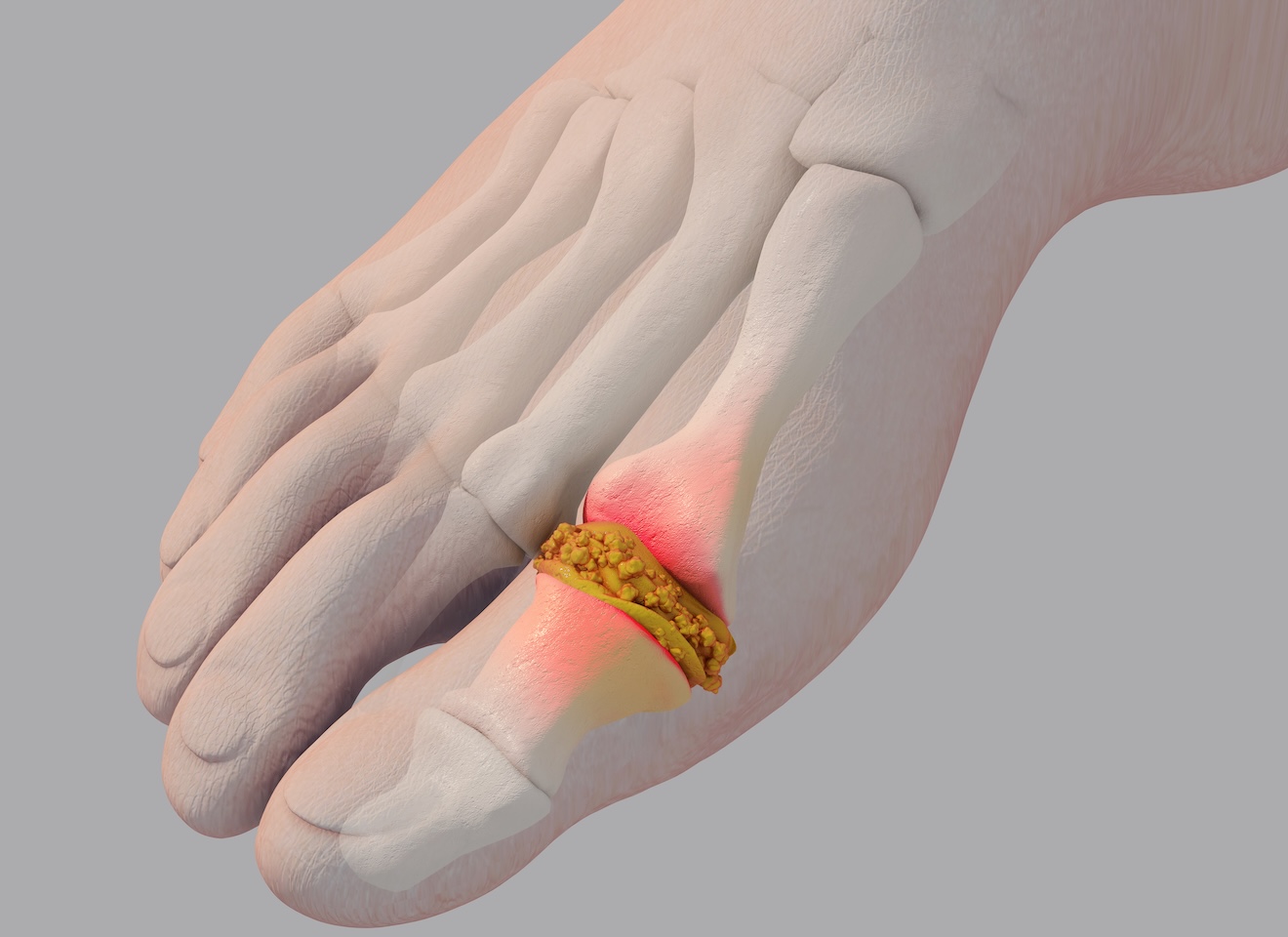
Early evaluation is important because gout can mimic a joint infection, which requires urgent treatment. The gold standard for diagnosing gout is an arthrocentesis, where a specialist uses a needle to withdraw a small amount of fluid from the inflamed joint. We examine the fluid under a microscope for the presence of uric acid crystals within white blood cells.
Identifying these crystals confirms the diagnosis and helps distinguish gout from infections or other forms of arthritis, which can present similarly but require different treatments. Blood tests may reveal elevated uric acid levels, though levels can be normal during an acute flare. In more advanced cases, we might use imaging to detect joint damage or crystal deposits.
A disease that’s shaped history
Few conditions have as rich a documented history as gout. Ancient Egyptian records dating back to 2640 B.C.E. describe symptoms consistent with gout of the big toe. The Greek physician Hippocrates in the 5th century B.C.E. called gout “the unwalkable disease” and noted its association with wealthy lifestyles.
The term "gout" emerged in the Middle Ages from the Latin word “gutta,” meaning "drop." At the time, physicians believed the pain was caused by a drop of one of the body’s “four humors” seeping into a joint, causing swelling and pain. English physician Benjamin Welles published the first medical book on gout in 1669: A Treatise of the Gout, or Joint-Evil.
Purine-rich diets of red meat and alcohol were accessible only to the powerful and privileged.
Notable sufferers include Alexander the Great, Christopher Columbus, Henry VIII, Isaac Newton, Benjamin Franklin, and Ludwig von Beethoven.
What are the treatment options for gout?
Treatment strategies focus on two goals: relieving acute pain during flares and preventing future attacks.
- Acute flares are typically treated with nonsteroidal anti-inflammatory drugs (NSAIDs), corticosteroids, or colchicine to reduce inflammation and pain. In cases where these medications are ineffective or contraindicated, we may consider targeted biologic therapies, such as interleukin-1 (IL-1) inhibitors, that block inflammatory pathways.
- For chronic gout, we aim to prevent future attacks and shrink tophi. Medications such as allopurinol lower the concentration of uric acid in the blood so that crystals can no longer form. For patients with severe or treatment-resistant gout, newer therapies can replicate the missing uricase enzyme, converting uric acid into a form that is easier to eliminate through urine.
Lifestyle counseling is key to long-term management. Patients learn that maintaining a healthy weight, reviewing medications that can raise uric acid, and moderating purine-heavy foods all support long-term control. The DASH diet, developed to reduce hypertension, has been proven to decrease uric acid levels and lower the risk of gout. Another option is a heart-healthy Mediterranean diet. However, diet changes alone are rarely sufficient; medication is often necessary to fully manage the disease.
Gout is a medical condition, not a label of an excessive lifestyle. With early diagnosis and consistent care, most patients achieve lasting symptom control and few long-term complications.
If you have gout symptoms or think you may be at risk, talk with your primary care provider or request an appointment with a rheumatologist. We can create a personalized treatment plan to help you regain a more active, pain-free life.
To talk with an expert about gout, make an appointment by calling 214-645-8300 or request an appointment online.