What Conditions Are Treated With Cardiac Ablation?
Cardiac ablation treats arrhythmias that are not being properly controlled by medications. Some types of arrhythmias can be life-threatening; others are annoying. The types of arrhythmias and other heart conditions we treat with cardiac ablation include:
- Atrial fibrillation: Abnormal heartbeat in the upper chamber of the heart that causes a rapid, irregular heart rhythm. Ablation stops the abnormal electrical activity of the pulmonary veins and has the potential to cure patients of their atrial fibrillation.
- Atrial flutter: Abnormal heart rhythm where the upper chambers of the heart (atria) beat very fast but in a regular pattern, which can cause the heart to pump less efficiently. Patients with typical atrial flutter can be cured with ablation with a 98% success rate.
- Supraventricular tachycardia: Fast heart rhythms in the upper chamber caused by abnormal tissue. They are regular and start and stop suddenly. They are usually curable with ablation.
- Ventricular tachycardia: Abnormal rhythm in the lower chambers of the heart, which often is life-threatening. They typically are regular and fast. These also can be cured with ablation.
- Ventricular fibrillation: Abnormal heartbeat that causes the heart to beat fast and causes fainting within 10 seconds. It can lead to death unless treated promptly. This type is not often treated with ablation.
What Should Patients Expect During Cardiac Ablation?
Pre-Procedure Details
The cardiac electrophysiologist provides specific instructions to the patient before the ablation procedure and explains risks such as bleeding, infection, and adverse reaction to anesthesia.
Patients also meet with the anesthesiologist the day of the surgery to review their medical history and to develop an anesthesia plan for the procedure. Patients should not eat after midnight the night before the surgery.
On the day of the surgery, a nurse reviews the patient’s chart to make sure there are no concerns.
The anesthesiologist then starts a local anesthesia IV, and the patient is taken to the operating room. The procedure begins once the anesthesia takes effect.
Procedure Details
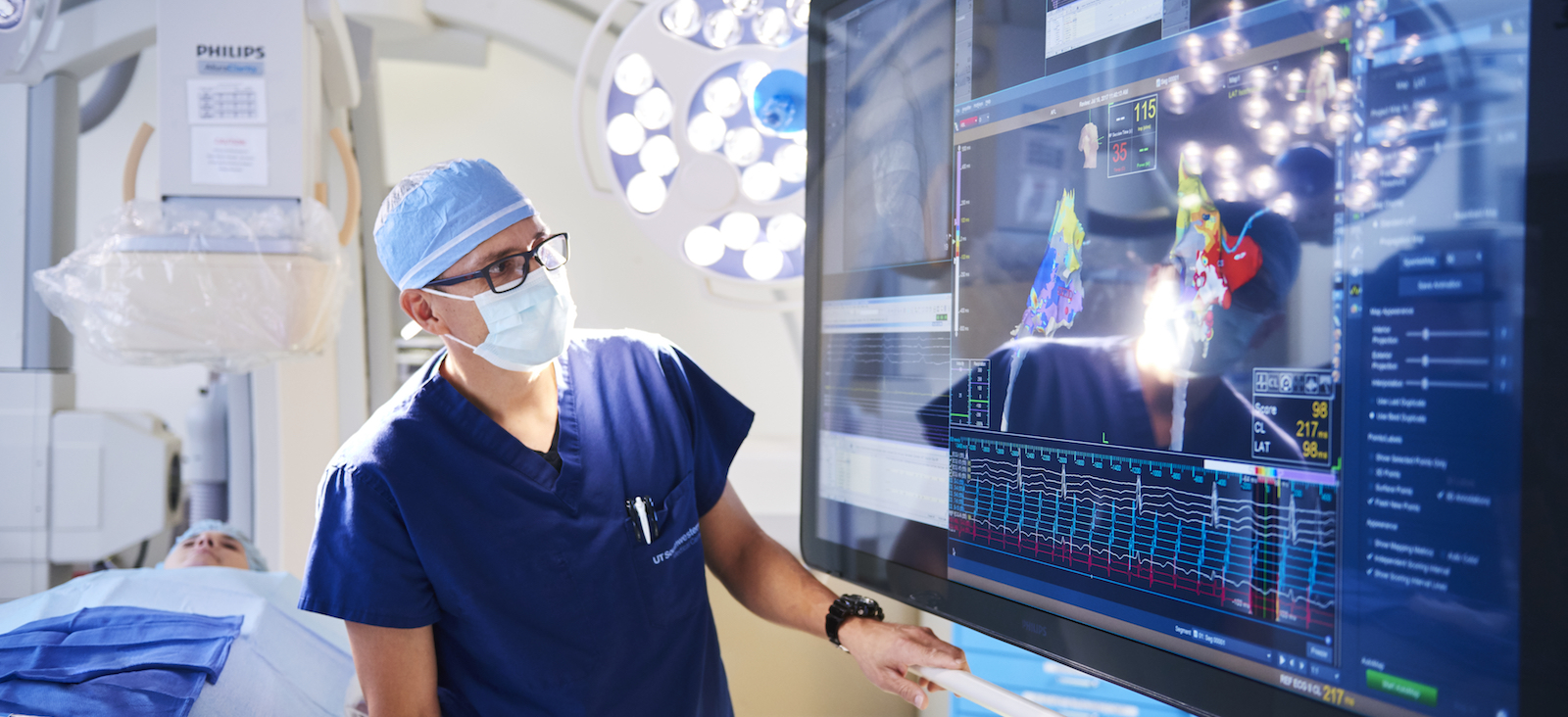
The cardiologist makes a tiny incision in the groin or wrist to access a vein or artery and inserts a thin, flexible tube (catheter). The cardiologist guides the catheter to the heart, then places small electrodes in various areas of the heart to find the source(s) of the irregular heartbeat. When the areas are located, the cardiologist uses the catheter to send heat or cold energy to the areas to scar or destroy them.
When the procedure is complete, all catheters and guidewires are removed, and the small incision is closed with manual pressure, stitches, or a special closure device.
Post-Procedure Details
After the procedure, patients are taken to the postoperative recovery area and monitored. Pain medication is given as needed. Most patients go home on the day of the procedure.
Some patients spend the night, particularly if their procedure is late in the day, if they live alone, or if they come from a distance.
Which Clinical Trials Are Available for Cardiac Ablation?
As one of the nation’s top academic medical centers, UT Southwestern offers a number of clinical trials aimed at improving the outcomes of patients with cardiovascular disease.
Our heart rhythm management team is involved in numerous trials of new treatments and devices, which means our patients have first access to novel technologies such as next-generation ablation devices, mapping systems, pacemakers, and defibrillators.