Restoring sensation and function with peripheral nerve surgery
March 2, 2023

Each of our hundreds of individual nerves has a particular job, controlling movement or sensation in specific parts of the body. The peripheral nerves – those outside the brain and spinal cord – carry motor and sensory signals that allow us to blink, high five, or tap our toes.
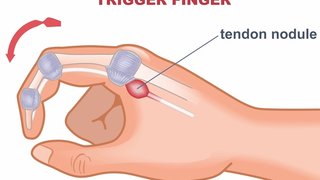
When one of our peripheral nerves is torn, separated, or compressed due to an injury, patients may lose sensation or movement in a muscle or limb. In some cases, nerve damage can cause symptoms such as pins and needles (neuropathy), pain, facial paralysis, migraines, or weakened or nonfunctioning muscles.
Peripheral nerve surgery may be able to restore part or all of these deficits when self-healing isn’t possible. But there is a limited window of time in which surgery might help.
Peripheral nerve surgery for loss of movement usually must occur within 9-12 months for the best chance at successful outcomes. Beyond that timeframe, the damage can be irreversible for reasons that researchers at UT Southwestern and around the world are working to understand.
Along with timely diagnosis, achieving good surgical outcomes relies on a wide range of clinical expertise. UTSW is one of the few centers in the region that can perform advanced peripheral nerve procedures – we have a deep bench of cross-functional nerve experts, including neurologists and neurosurgeons, rehabilitation medicine and pain management experts, plastic surgeons, orthopedic surgeons, hand surgeons, radiologists, and occupational and physical therapists.
Our team has an excellent track record of successful peripheral nerve surgery outcomes. Patients have regained function after severe nerve injuries through advanced treatments that may include medication, rehabilitation, and surgery.
Part of this success is because we recommend peripheral nerve surgery only when a patient’s exam, imaging, and functional tests show that positive outcomes are possible – and only when the timeline is right.
When peripheral nerve surgery might help
The physical exam after a traumatic injury such as a fall, severe joint dislocation, or vehicle accident is the starting point for assessing nerve damage. Regular MRIs can show areas where muscles and tendons are injured or inflamed, which means nerve damage might be part of the trauma.
However, specialized nerve imaging and testing gets us as close as possible to predicting a patient’s potential outcomes after surgery. Some peripheral nerve injuries heal without treatment, and some respond better to therapeutic exercise or medication. Making the distinction is a specialized skillset that requires insights from nerve experts in a range of disciplines.
Advanced imaging, such as magnetic resonance neurogram (MRN), can show us detailed images of the nerves, whereas regular MRIs focus on the muscles and joints. Our radiologists are experts in interpreting these images. Pairing their skill with our specialized understanding of how peripheral nerves function, we can gain a more precise picture of whether surgery might restore sensation or movement.
For example, if we can see that a nerve is severed or excessively stretched or torn, we know self-healing is not possible and surgery may be a good option.
Along with imaging, we may also order an electrodiagnostic study to determine how well a damaged nerve is functioning. Our colleagues in neurology administer and interpret these tests, which can tell us whether a peripheral nerve is being compressed or how badly it is injured. In either situation, the nerves likely will not fully heal on their own and may require surgery.
Our team of specialists discusses each patient’s imaging and testing to determine whether surgery is appropriate. We talk through every option available to a patient to help set realistic expectations about regaining function.
Related reading: Too gruesome for video: The ‘high-energy’ injury of Dallas Cowboy Allen Hurns
'Our team has an excellent track record of successful peripheral nerve surgery outcomes. Patients have regained function after severe nerve injuries through advanced treatments that may include medication, rehabilitation, and surgery.'
Jonathan Cheng, M.D.
What to expect with peripheral nerve surgery
Though many of the motor and sensory nerves are small – some as thin as dental floss – we may need to make larger surgical incisions depending on their location.
For example, if we need to access the brachial plexus – nerves that exit the spinal cord and extend from the shoulders to the fingertips to control movement – we may need to make 3- to 4-inch, or longer, surgical incisions. Our plastic surgeons use the latest techniques to minimize incision length and scarring whenever possible.
Peripheral nerve surgeries may involve moving or removing bone and tissue along with nerves, and we work as a team to get the best outcomes for patients. Some of the peripheral nerve procedures we perform include:
- Decompression: Releasing a nerve that is either “pinched” by surrounding tissue or pinned against a muscle, bone, or tendon. This is an effective treatment for carpal tunnel syndrome and some types of migraines.
- Reconstruction: Repairing and rebuilding damaged nerves, such as reattaching the ends of a nerve that has been severed.
- Nerve transfer or graft: Moving a healthy nerve from one area of the body to the injury site with the hope it will flourish and resume the damaged nerve’s job.
- Tendon or muscle transfers: A section of healthy muscle or tendon is moved from another area of the body and secured in the damaged area with the goal of functional restoration.
- Revision: Repairing incomplete recovery after a previous surgery performed elsewhere.
In our research lab, we are developing techniques to increase our ability to resupply the muscles with nerves. In this way, we can optimize recovery of nerves and muscle tissue, maximizing function after reconstruction.
Related reading: What's causing ‘electric’ facial pain? It might be trigeminal nerve damage
Recovering from peripheral nerve surgery
Depending on your condition, surgery site, and procedure, you may be able to resume some daily activities within a few days. However, it can take several months for the nerves to fully heal.
If you have been living with mobility deficits, you may need ongoing therapy with our physical medicine and rehabilitation (PM&R) team. PM&R therapists can help you regain strength and function to areas weakened by damaged nerves.
It is possible in some cases to restore function and sensation over time. Less extensive injuries typically offer a better chance at full recovery. However, some nerve injuries are too widespread or severe to be reversed, and patients will have permanent deficits.
Fortunately, advanced treatment options can help patients manage pain symptoms and reduced function:
- Nerve-targeting medications can control pain and increase function.
- Nerve block injections can prevent the nerve from sending and receiving sensory signals, reducing discomfort.
- Occupational and physical therapy can prevent and reduce stiffness, and patients can learn new or different movements to perform daily tasks.
Managing a peripheral nerve injury is a team effort. UT Southwestern’s team of specialists works together to personalize treatment plans, and we have an excellent record of achieving good outcomes for our patients.
Researchers, including some in our labs, continue to make advances in understanding the nerve-to-muscle connection and time-sensitivity of surgery. As new connections are made, we can offer patients even more precise treatments.
To explore peripheral nerve surgery options, call 214-645-8300 or request an appointment online.