Expertise in Vascular Access
Vascular access is a method of catheterization that provides a convenient method to repeatedly draw blood from or deliver medication to a patient’s bloodstream.
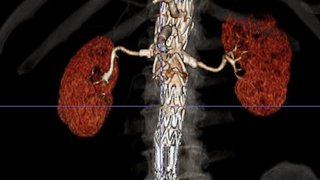
Vascular access devices include port-a-cath, tunneled dialysis, pheresis catheters, and peripherally inserted central catheter (PICC) lines. To place these devices, interventional radiologists insert a flexible, sterile, thin plastic tube, or catheter, into a large vein in the neck (internal jugular vein), chest (subclavian vein), or groin (femoral vein).
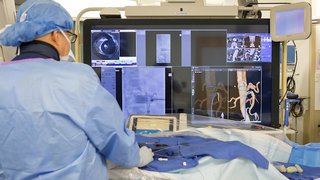
Our interventional radiologists specialize in catheter placements and treatment of the areas of the body involved.
In addition to the training that all radiologists receive, these specialists have advanced fellowship training in interventional radiology, plus extensive real-world experience.
Our team of interventional radiologists and physician assistants coordinates each patient’s complete care – from imaging evaluation to post-procedure follow-up – maintaining a high level of communication throughout the process.
In addition, we coordinate closely with experts from across the UT Southwestern community when necessary.
Uses for Vascular Access
Some common uses of central venous catheters include:
- Blood transfusions
- Chemotherapy
- Hemodialysis
- Intravenous antibiotic therapy
- Intravenous medications
- Long-term intravenous feeding for nutritional support
- Photopheresis
- Plasmapheresis
- Improvement of venous access
Catheters can stay in place from days to years, depending on the needs of each patient. Once the catheter is no longer needed, it can easily be removed at the clinic under sterile conditions and a local anesthetic.
Preparing for Catheter Placements
Catheter placements are performed with conscious sedation, a process in which the patient is given medication to feel sleepy but is not unconscious. Conscious sedation requires that the patient fasts for eight hours before the procedure.
Most medications can be taken the morning of the procedure except for medications that affect blood clotting, such as aspirin, Plavix, Lovenox, or Coumadin. Patients who are taking one of these medications might need to stop taking it or be switched to another medicine for a few days before the procedure. Our team will coordinate the patient’s medication management, if necessary.
What to Expect After Catheter Placement
Catheter placement procedures are performed by a professional interventional radiology team, consisting of a physician, a technician, and a nurse in a sterile, surgical environment. After the procedure, the patient will be given instructions describing care for the catheter.
The patient should anticipate some discomfort following the procedure, but the pain is generally controlled with over-the- counter medication.