Male infertility: Treating the physical and emotional side effects
August 11, 2022

One out of eight couples has difficulty getting pregnant, and in 30% of male/female couples with infertility or subfertility, the male partner has the complication. (In 30% the woman does, and in 30% it is a combination of both partners.)
But men are often reluctant to seek treatment or even talk about fertility with their doctor.
Growing up, many men have been taught the myth of absolute male fertility – presuming that they’d be able to father a child at any age. Some even believe there is a relationship between fertility and masculinity. (There isn’t.) When confronted with a subfertility or infertility diagnosis, they can feel frustrated, disappointed, and lost. Others may feel inclined to “tough it out” or internalize their emotions.
Health care providers also tend to underestimate male factor infertility. Only about 40% of Ob/Gyns recommend a urological evaluation for the male partner if a couple is struggling to conceive, according to a study by RESOLVE: The National Infertility Association.
At the UT Southwestern Male Infertility Clinic, we take a personalized approach to determining what is causing subfertility or infertility in our patients – whether it’s structural conditions, sperm production, hormonal or genetic disorders, or lifestyle factors.
We provide patients with access to leading-edge therapies to help preserve and restore their fertility, working collaboratively with reproductive endocrinologists to enhance the couple’s care and put them on the path to parenthood.
The first step for most men, however, is to consider they might have a fertility problem and to seek care from a specialist.
Potential causes of male infertility
Male infertility has many causes, including low or no sperm production, abnormal sperm function, or blockages that prevent delivery of sperm.
Common factors that contribute to male infertility include:
- Genetic disorders such as cystic fibrosis, hemochromatosis, chromosomal abnormalities, or Klinefelter’s or Noonan syndromes
- Hormonal disorders
- Defects in the tubes that carry sperm, leading to blockages
- Cancer treatment, such as radiation and chemotherapy, which can cause short- or long-term male infertility
- Certain medications including testosterone replacement therapy, long-term anabolic steroid use, and some ulcer and arthritis drugs
- Exposure to heavy metals or toxins
- Obesity or being overweight
- Tobacco and heavy alcohol use
Related reading: How low testosterone treatment can help – and harm – a man's sex drive and fertility
In the U.S., more people are waiting longer to get married –the average age for women in Texas is 26.6 and for men it’s 28.5. Nationally, the average age for a first pregnancy has increased to 26.3. These are contributing factors to higher rates of infertility. It is fairly well known that fertility declines after age 35 for women, but many men are not aware that with age, both sperm count and movement (motility) decrease.
At UT Southwestern, we provide patients with a thorough evaluation that includes capturing a detailed personal and medical history. Often, we’re able to identify some potential causes of subfertility and infertility in the initial exam.
We’ll also conduct a semen analysis, which will measure the patient’s sperm volume, motility, and shape (morphology). Based on those results, we may also recommend genetic and hormonal testing to further diagnose the root cause of the subfertility and develop a personalized treatment plan.
How we treat male infertility
Male infertility diagnoses tend to break down into three categories: Obstructive, nonobstructive, and idiopathic, which means the cause cannot be identified (about 10% of cases).
Depending on the diagnosis, we offer multiple treatment options, ranging from medication to microsurgery to retrieve sperm.
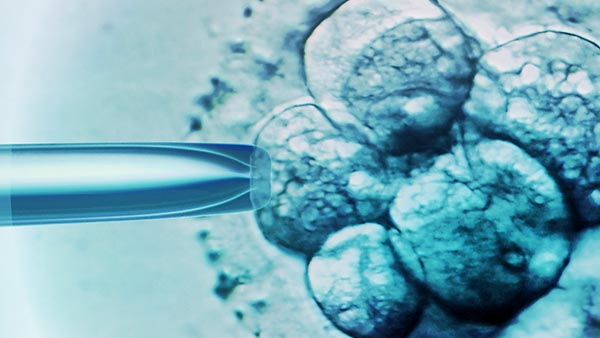
For structural blockages in the epididymis (a tube behind the testicle) or vas deferens (the tubes that move sperm from the testicles to the urethra), we may be able to repair the obstruction with microsurgery or retrieve sperm directly from the testicles or epididymis. The sperm extracted from the testicle can be used only for in vitro fertilization to achieve pregnancy.
For hormonal problems, such as low testosterone, medication prescribed and administered by a specialist can be effective for some patients. However, taking exogenous (synthetic) testosterone or over-the-counter supplements may decrease fertility if not administered properly.
Natural testosterone and sperm production is fueled by two hormones created in the pituitary gland of the brain: luteinizing hormone (LH) and follicle-stimulating hormone (FSH). When a man takes synthetic testosterone, the brain detects the excess and slows or stops production of LH and FSH. That means the body quits producing intratesticular (natural) testosterone and, consequently, production of sperm due to the suppression of LH and FSH. This results in reduced fertility.
Talk with your doctor if you think you have low testosterone. Taking testosterone supplements directly, such as injections, can lead to reduced or completely discontinued sperm production.
Genetic diseases such as Klinefelter’s syndrome, in which males are born with an extra sex chromosome in their cells, may lead to low or no sperm production. In patients with no sperm production, we may be able to extract sperm through microscopic testicular sperm extraction. In this procedure, we remove a small amount of testicular tissue, which is examined under a microscope to look for sperm.
If sperm are present, we can use them right away via in vitro fertilization to fertilize an egg or freeze the tissue to potentially extract sperm in the future. Approximately 40-50% of patients with no sperm production can benefit from this procedure.
Erectile dysfunction or premature ejaculation can interfere with physical and emotional intimacy. Medication or counseling can be effective for these conditions.
Related reading: Fertility options for cancer survivors
Infertility affects more than just your physical health
Research has shown that people who struggle with infertility can experience similar levels of anxiety and depression as patients with cancer or heart disease.
Along with multiple doctors’ appointments, tests, and procedures, and dealing with insurance companies, you and your partner may also be dealing with loved ones who pester you about when you’re going to have children. Oftentimes, they offer unsolicited and incorrect advice on ways to improve your chances of conceiving.
These situations can be particularly challenging for men, some of whom have been taught there is a relationship between fertility and masculinity. (There isn’t.) Women’s infertility is often viewed as a more tragic and emotional situation, and therefore it’s more likely to be discussed and supported among friends and family.
Unfortunately, stress and depression associated with infertility can compound the problem. It’s hard to function and feel normal in a sad or anxious state, let alone have the energy for sex. And it’s not uncommon for men to experience low libido or erectile dysfunction while dealing with infertility issues.
As part of our treatment in the Male Infertility Clinic, we refer many patients to therapy to work through the emotional challenges of subfertility. In some cases, getting to the root of mental health symptoms can improve fertility without further treatment.
The future of male infertility research, treatment
In addition to the advanced treatment options we already offer patients, promising research is underway that may help shape the future of male factor infertility treatments.
For instance, researchers in Canada recently used a 3D printer to create viable testicular cells from a patient who was suffering from nonobstructive azoospermia (no sperm in the semen), or NOA, a condition that causes a sperm production problem in the testicle. The lab at the University of British Columbia collected stem cells from a biopsy of the patient’s testicles and cultured them and 3D-printed them onto a petri dish. The next step, which will likely take several years of additional research, will be to train the printed cells to produce actual sperm.
At the University of Pittsburgh, scientists are conducting research that could help prepubertal patients who are facing cancer treatments or who suffer from genetic conditions such as Klinefelter’s syndrome maintain future fertility. Because prepubescent boys are too young to produce sperm, researchers are exploring the viability of freezing testicular tissue as a way to preserve their fertility.
The hope is that the thawed spermatogonial stem cells in the tissue can be matured to produce functional sperm. Studies in other mammals have produced sperm from frozen prepubertal testicular tissues. Our colleagues at Children’s Health in Dallas have joined the University of Pittsburgh in these efforts.
One of the biggest challenges in trying to develop the next generation of treatments for male infertility is that human sperm cells are fragile and don’t live long outside the body. That’s why the field of sperm cryopreservation continues to be a first-line procedure for many men facing medical conditions or treatments that could affect their fertility.
There also has been an increase in healthy young men, ages 18-25, who are choosing to freeze their sperm. They want to wait to have children, but because sperm quality diminishes with age, they’re opting to retain their fertility through sperm cryopreservation.
At UT Southwestern’s Male Infertility Clinic, we understand the physical and emotional challenges that come with a diagnosis of subfertility and infertility. But we’re also equipped to offer patients the latest and most effective treatment options to restore and preserve fertility.
To talk with a male fertility specialist, call 214-645-8300 or request an appointment online.










