Refining Stereotactic Body Radiation Therapy for Breast Cancer
October 2, 2020
Clinical Trials at UT Southwestern
For referring or potentially referring physicians and the public, we have an excellent resource for rapid inquiries. To learn more about our breast cancer clinical trials and eligibility, please email us. You can also find more detail by searching clinicaltrials.gov.
At the Harold C. Simmons Comprehensive Cancer Center at UT Southwestern we are proud to be the first center in Texas and the second center in the world to offer our patients with breast cancer GammaPod (Xcision Medical Systems, Columbia, Maryland) as a treatment option.
While standard whole breast irradiation can require daily treatments for three to six weeks, partial breast radiation treatment with GammaPod can be as short as one to five days. In addition to enhanced patient convenience, shortening radiation courses is even more important in the era of COVID-19. This platform allows us to minimize the number of trips to the radiation oncology suite and thus minimize potential virus exposure for patients, while striving to improve their outcomes.
What Is GammaPod?
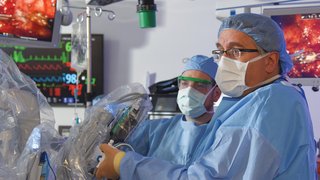
GammaPod is a Food and Drug Administration-approved stereotactic radiation machine that allows practitioners to pinpoint and treat breast cancer. When patients are treated with GammaPod, they are situated on a patient-loading couch in a prone position, which helps limit the dose of radiation to the skin, heart, and lungs. Unlike any other stereotactic body radiation therapy (SBRT) machine, GammaPod is equipped with a vacuum-assisted breast immobilization cup with an embedded fiducial wire that keeps the target centered during treatment. With the patient in position, the couch can be loaded directly onto a CT table for scanning, minimizing error between target localization and subsequent delivery of the prescribed dose.
With GammaPod, we can administer higher doses of radiation in a more controlled and patient-friendly manner compared with conventional treatments. After CT localization, the cup-based coordinate system of GammaPod delivers treatment from a multisource Cobalt-60 stereotactic radiotherapy system. This system uses 25 cobalt sources of radiation that continuously rotate during treatment, creating thousands of beam angles that converge at the target to create an intense focal spot. This means we can achieve reduced treatment margins (2–3 mm) compared with those required by conventional radiation therapy (10–15 mm). Thus, the target, either the cavity of the tumor or the tumor itself, receives a full dose while the surrounding healthy tissue is spared.
“Advances in SBRT are yielding more convenient treatment regimens for patients and decreased toxicity to tissue surrounding the treatment area.”
Asal Rahimi, M.D.Director of Clinical Research
Our GammaPod Clinical Trials
We have multiple ongoing clinical trials with GammaPod: a phase one preoperative radiation dose escalation (toward an ablative dose) study of single-fraction stereotactic partial breast radiotherapy (NCT04040569); a phase two trial evaluating health-related quality of life and cosmesis after five-fraction stereotactic partial breast irradiation (NCT03581136); and a single-arm study to assess patient-level adverse-event and tumor outcomes after receiving a post-lumpectomy tumor bed boost with the GammaPod followed by whole breast radiation (NCT03562273).
In our preoperative single-fraction radiation trial (NCT04040569), we will give one treatment of radiation prior to surgery. Preoperative radiation can minimize the amount of tissue that is ultimately irradiated, in comparison to radiation after surgery. Other advantages are that we might be able to deliver an ablative dose and eliminate the tumor with a single fraction of radiation. Furthermore, in collaboration with our Radiology, Translational Medicine, and Physics departments, we are exploring the relationships between imaging techniques and predictions for patient and tumor responses.
Expanding Use of GammaPod
I am Co-Chair of the GammaPod Consortium, which includes a growing community of institutions that are committed to exploring new clinical applications and developing clinical protocols to treat breast cancer with GammaPod. The GammaPod Consortium helps current and new member institutions launch and develop their GammaPod-based research programs and brings together all the consortium members to coordinate and conduct multi-institutional clinical trials. Current member institutions are the University of Maryland School of Medicine in Baltimore, UT Southwestern Medical Center in Dallas, Alleghany General Hospital in Pittsburgh, and The Ottawa Hospital Cancer Centre in Canada.
Advances in SBRT are yielding more convenient treatment regimens for patients and decreased toxicity to tissue surrounding the treatment area. Furthermore, with fewer treatments, SBRT might be more cost-effective than conventional radiation therapy, where each day of treatment is associated with added costs for the health care facility and the patient.
Future studies with GammaPod will likely examine a single fraction of radiation treatment and incorporate real-time imaging, such as magnetic resonance-based localization, to guide treatment for seamless targeting. SBRT systems have emerged as a promising option for breast cancer treatment and will continue to be refined to limit toxicity and improve patient outcomes.