Writing Her Own Story: Breast Cancer Survivor Angela Sells
August 1, 2022
To learn more about our breast cancer clinical trials and eligibility, please email us. You can also find more detail by searching clinicaltrials.gov.
A patient with HER2-positive breast cancer received personalized care with the help of clinical trials. Now, she’s advocating for more participation in research.
On Oct. 6, 2020, the 25th anniversary of her mother’s death from breast cancer, Angela Sells was diagnosed with stage 2 HER2 (human epidermal growth factor receptor 2)-positive breast cancer. She was 64 years old. “Having a family history of breast cancer, I have always been dutiful about getting mammograms,” Angela says. “I think I’ve always kind of anticipated that I might be diagnosed, but I didn’t realize how afraid I was of that diagnosis until I got it.
“I immediately asked for a referral to UT Southwestern. It’s a National Cancer Institute-designated cancer center, and I wanted the academics and the research and the clinical practice that go along with the cancer treatment available there,” Angela recalls.
At Harold C. Simmons Comprehensive Cancer Center, she met with Deborah Farr, M.D., an Associate Professor of Surgery in the Division of Surgical Oncology, who specializes in the surgical treatment of breast cancer. “For her type of cancer, the standard of care is to do chemotherapy with anti-HER2 therapy before surgery. Whether or not the patient participates in a clinical trial depends on if they’re eligible for the trial and if they’re willing to participate in the trial,” says Dr. Farr, who subsequently referred Angela to Simmons Cancer Center medical oncologist Sangeetha Reddy, M.D., Assistant Professor of Internal Medicine in the Division of Hematology-Oncology.
With the four-drug standard-of-care treatment, patients with HER2-positive breast cancer have experienced significant improvement in outcomes. “However, in some patients, the cancer comes back,” Dr. Reddy explains. “In other patients, we may be treating too much. Potential adverse events include long-term neuropathy, impacts on the bone marrow, and increased risk of infection.
“I am very passionate about people in clinical trials now. I would like to help alleviate some people’s fears around clinical trials.”
Angela Sells
“We are working to personalize anti-cancer treatment to each individual patient,” Dr. Reddy adds. “On the one hand, we are hoping to de-escalate treatment of cancers that can be effectively treated with fewer therapies, while at the same time we are offering newer options for cancers where our current therapies are inadequate. For de-escalation trials, the goal is to maintain clinical outcomes, while at the same time decreasing toxicity and sparing patients from the adverse events associated with the four-drug treatment.”
“I got somewhat lucky,” Angela says. “I was diagnosed in October, and they had just started a clinical trial for my particular subtype of breast cancer in September.”
The phase 2 clinical trial, called CompassHER2-pCR, is evaluating the safety and efficacy of reducing the number and duration of chemotherapies given alongside HER2-targeted therapies to patients prior to surgical treatment of their HER2-positive stage 2-3a breast cancer.
“Dr. Reddy assured me,” Angela says. “‘It has been 25 years – your story and your mother’s story are very different.’”
Angela began treatment on Nov. 10, 2020, and by January 2022 she achieved a pathological complete response with limited side effects. “I am filled with gratitude every day because I am so lucky to be here,” she says.
“One of Simmons Cancer Center’s biggest strengths is our clinical trials, and another is our reconstructive surgeons and capabilities to do autologous tissue transfer for breast reconstruction,” Dr. Farr says. “Following her medical oncology treatment, Angela had a double mastectomy performed by myself and Dr. Nicholas Haddock, who then performed her breast reconstruction surgery.”
“I am very passionate about people in clinical trials now,” says Angela, who was invited to be part of an inaugural research advocacy group at UT Southwestern. “I would like to help alleviate some people’s fears around clinical trials. As an experienced nurse, I think I can help translate the medical terminology for patients considering trials. A trial may not work for everybody, but I hope they will at least consider them.
“In addition to the CompassHER2-pCR trial, we are also enrolling in clinical trials across the different types of breast cancer in both localized and metastatic disease so that we can maximally help our patients,” Dr. Reddy says. Included are trials that were first developed at UT Southwestern, such as a new immunotherapy and chemotherapy combination that can kick-start an individual’s own immune response against the cancer in cases of metastatic triple negative breast cancer (NCT05029999).
Metabolic Pathways May Represent New Therapeutic Target in Metastatic Cancer
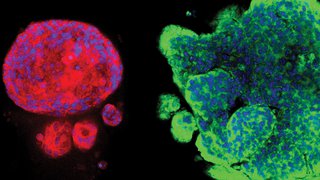
In a project co-led by Harold C. Simmons Comprehensive Cancer Center researchers Srinivas Malladi, Ph.D., and Pravat Kumar Parida, Ph.D., a team at UTSW has discovered significant diversity in the metabolism of different types of metastatic HER2+ breast cancer cells. The findings, published in Cell Metabolism, highlight metabolic vulnerabilities in malignant cells that could eventually be targeted with new cancer therapies.
About half of patients with HER2+ breast cancers develop secondary tumors, with the brain being a common site for breast cancer metastasis. These brain metastases may be diagnosed at the same time as the primary breast tumor, known as synchronous brain metastasis (S-BM), or after the primary breast tumor diagnosis, known as metachronous brain metastasis (M-BM). S-BMs are rarer and have worse prognoses than M-BMs. Patients may also develop latent brain metastases that are asymptomatic and can lead to M-BM over time.
Using an animal model, the researchers found significant differences in the metabolism of these different types of metastatic cells. For example, S-BM cells used glucose as a primary fuel source, while M-BM and latent cells used the amino acid glutamine. Also, compared with latent cells, M-BM and S-BM cells secreted more lactate, which helps these malignant cells evade innate immune surveillance.
The researchers also found elevated levels of a protein known as xCT, which mediates oxidative stress, in the M-BM and latent cells compared with primary tumor cells. Inhibiting the activity of this protein significantly reduced the metastatic activity of M-BM and latent cells and made them more vulnerable to drugs that target HER2+ cells.
Reference: Parida PK, Marquez-Palencia M, Nair V, et al. Metabolic diversity within breast cancer brain-tropic cells determines metastatic fitness. Cell Metab. 2022;34(1):90-105.e7. doi:10.1016/j. cmet.2021.12.001