- Texas Medical Association
- American Head and Neck Society
- American College of Surgeons
- American Association for Cancer Research
- American Academy of Otolaryngology - Head & Neck Surgery

Baran Sumer, M.D.
- T.C. Lupton Family Professorship in Patient Care, in Honor of Dr. John Dowling McConnell and Dr. David Andrew Pistenmaa
- Otolaryngology
- Head & Neck Cancers
- Transoral Robotic Surgery
New Patient Appointment Accepting Virtual Visits or 214-645-8898
Biography
Baran Sumer, M.D., is Professor and Chief of the Division of Head and Neck Oncology in UT Southwestern Medical Center's Department of Otolaryngology, where he has served on the faculty since 2007. A specialist in head and neck cancer surgery and reconstruction, Dr. Sumer is also Director of the Head and Neck Oncology Disease Oriented Team at Simmons Comprehensive Cancer Center and holds the T.C. Lupton Family Professorship in Patient Care. He was also the inaugural Program Director for the Head and Neck Oncology and Microvascular Reconstructive Surgery Fellowship.
Dr. Sumer earned his medical degree at Case Western Reserve University. He then completed an internship in general surgery, a residency in otolaryngology, and a fellowship in head and neck oncologic surgery and microvascular reconstruction at Washington University School of Medicine in St. Louis.
Dr. Sumer serves on committees for NRG Oncology, the American Head and Neck Society (AHNS), and the World Molecular Imaging Society (WMIS) and served as a permanent member of the Innovations in Nanosystems and Nanotechnology (INN) study section (formerly NANO) for the National Institutes of Health (NIH) Center for Scientific Review between 2020-2024.
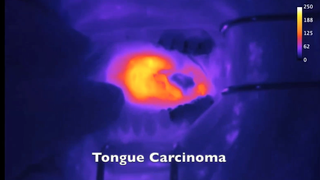
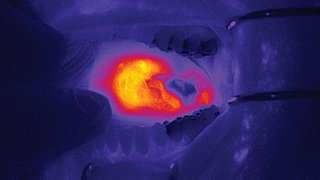
He has participated in a wide variety of research studies devoted to advancing diagnostic and therapeutic techniques and technologies for head and neck cancer, such as fluorescent imaging, biosensing, hyperspectral imaging, photodynamic therapy, and image-guided surgery.
His collaboration with another UT Southwestern faculty member, Jinming Gao, Ph.D., has led to several inventions in their joint lab, including a pH-sensitive nanoparticle that can be used to deliver therapeutics and imaging agents specifically to cancers. Drs. Sumer and Gao's work with the pH nanosensor has resulted in a European phase 1 clinical trial, completed in 2019, and a phase 2 clinical trial in the U.S. for cancer patients with peritoneal metastases, completed in 2023.
The fluorescent nanoparticle they co-developed for these clinical trials illuminates cancer cells during surgery, potentially allowing surgeons to visualize the tumors more accurately. This nanoparticle, pegsitacianine (ONM100), is manufactured by OncoNano Medicine, a biotechnology company co-founded by Dr. Sumer and Dr. Gao.
Dr. Sumer is currently the PI of another phase 2 clinical trial, the ILLUMINATE trial, which is testing the ability of pegsitacianine to identify unknown primary cancers of the head and neck and to fluorescently label head and neck cancers undergoing robotic surgery. The ILLUMINATE trial is funded by a R01 grant from the NCI.
Among numerous recognitions, honors, and awards, Dr. Sumer has been recognized as among the best otolaryngology physicians in North Texas by D Magazine. He is also the recipient of a Texas Instruments Corporate Award Research Gift, the Triological Society Francis Lederer FUSION Grant for Nanotechnology Research, and the SEBM Best Paper Award in the Alan MacDiarmid Interdisciplinary Research Society for Experimental Biology and Medicine.
Dr. Sumer serves as principal investigator and co-investigator on several research projects funded by the National Institutes of Health (NIH) and the National Cancer Institute (NCI).
Meet Dr. Sumer
Head and Neck Cancer Specialist in Dallas
The head and neck have many critical blood vessels, nerves, and structures that affect appearance as well as key functions such as speaking and swallowing. Because of the skill required to treat cancers in this area, patients with head and neck cancer should seek experts with mastery of the most recent treatments.
Otolaryngologist Baran Sumer, M.D., leads a team of head and neck cancer experts at UT Southwestern Medical Center offering the latest therapies, including minimally invasive surgical techniques and targeted radiation and chemotherapy.
Thanks to the latest advances in robotic surgery, many head and neck cancers can be removed with minimal damage to healthy tissues.
“These procedures tend to be much better tolerated by patients than surgery in the past, which would often result in problems with swallowing and speech,” Dr. Sumer says. “We perform endoscopic and robotic procedures that allow us to go through the mouth, requiring no incisions on the outside of a patient’s neck or face.”
A D Magazine Best Doctor, Dr. Sumer has a special focus on transoral robotic procedures (TORS) and laser procedures. Dr. Sumer made medical history in North Texas when he became the first surgeon in the region to perform a TORS procedure to remove a throat malignancy. A multi-year, multi-institutional study, E3311, published in the Journal of Clinical Oncology in 2022, has shown that TORS can safely reduce the amount of chemotherapy and radiation for patients with resectable p16+ locally advanced oropharynx cancer.
Comprehensive, multidisciplinary care
In addition to surgical, radiation, and medical oncologists, UT Southwestern’s head and neck cancer team includes plastic reconstructive surgeons, speech pathologists, orthodontists, oral surgeons, nutritionists, and physical and occupational therapists.
“Physicians do play an important role in the treatment of head and neck cancer,” Dr. Sumer says, “but it’s the multidisciplinary care, counseling, and rehabilitation our team offers that ultimately allow patients to achieve the best quality of life.”
The benefits of this collaborative approach to treatment of these complex cancers are seen every day at UT Southwestern.
“We’ve had patients who were told by other physicians that they would need their entire tongues removed, or that they would need a hole in their neck to breathe through for the rest of their lives,” Dr. Sumer says. “We were able to cure their malignancies and preserve their swallowing and speech. You can imagine how important that is, not only for people whose livelihoods involve speaking, but for everyday activities that we otherwise tend to take for granted.
“I have had many patients return to thank me, saying, ‘I can go out to restaurants and enjoy eating dinner in public with my family and friends.’ That's a very rewarding feeling.”
Education & Training
- Fellowship - Washington University in St. Louis School of Medicine (2006-2007), Head & Neck Oncologic Surgery
- Residency - Washington University in St. Louis School of Medicine (2002-2006), Otolaryngology
- Internship - Washington University in St. Louis School of Medicine (2001-2002), General Surgery
- Medical School - Case Western Reserve University School of Medicine (1997-2001)
Professional Associations & Affiliations
Honors & Awards
- AAO-HNSF 2019 Annual Meeting 2019, Honorary Guest Lecture: H. Bryan Neel III MD, PhD Distinguished Research
- Winner Lloyd Storrs Resident Award (Mentor) 2015, Teaching
- Alan MacDiarmid Interdisciplinary Research- Society for Experimental Biology and Medicine 2014
- Triological Society Francis Lederer 2011, FUSION Grant for Nanotechnology Research
- University of Texas Southwestern Medical Center, Department of Clinical Sciences 2008, Research Grant
- Texas Instruments Corporate Award 2008, Research Grant
- American Academy of Otolaryngology-Head and Neck Surgery 2008, Research Award
Books & Publications
-
Books
-
Theranostic Polymeric Micelles for Cancer Imaging and Therapy, in Multifunctional Nanoparticles for Drug Delivery Applications
Huang G, Khemtong C, Bey EA, Boothman DA, Sumer BD, Gao J. (257-276 (2012).), Svenson S, Prod?homme R.K. Springer Science & Business Media, Inc -
Clinical Applications of Heme Biosynthetic Pathway: Photodynamic Therapy with Protoporphyrin IX in Heme Biology: The Secret Life of Heme in Regulating Diverse Biological Processes
Ding H, Sumer BD, Gao J (2011) -
Oral Cavity Cancer in Decision-Making in Plastic Surgery
Sumer BD, Myers LL (2010), Quality Medical Publishing -
Vestibular Physiology
Goebel JA, Sumer BD (2006), New York, Theme Publishers -
Neck Dissection and Parotidectomy for Melanoma in Cutaneous Melanoma
Charles M. Balch, Michael B. Atkins, Claus Garbe, Jeffrey E. Gershenwald, Allan C. Halpern, John M. Kirkwood, Grant A. McArthur, John F. Thompson, Arthur J. Sober ( https://doi.org/10.1007/978-3-030-05070-2, 2020)
-
Theranostic Polymeric Micelles for Cancer Imaging and Therapy, in Multifunctional Nanoparticles for Drug Delivery Applications
-
Publications
-
Supportive Care Needs Among Pretreatment Head and Neck Cancer Patients According to Smoking Status: A Cross-Sectional Study With Nested Analyses
Mitchell DN, Jefferson A, Pyne J, Ho A, Iyer AG, Sumer BD, Balis D, Kumar S, Schnoll R, Day AT Laryngoscope investigative otolaryngology 2026 Feb 11 -
Body Mass Index and Nutritional Status With Immunotherapy Response in Head and Neck Cancer
Gabra L, Nitsch A, Wang Y, Liu Y, Truelson JM, Myers LL, Tillman B, Day A, Stankova L, Moon DH, Sher D, Farzal Z, Swiatowiec N, Hughes RS, Cao Y, Sumer BD JAMA Otolaryngology - Head and Neck Surgery 2026 -
Single-Operator Cancer Vision Goggles for Quantitative Near-Infrared Fluorescence-Guided Oncologic Surgery
Xu X, Zhang H, Ta C, Zurutuza I, Blasi N, Gautam KS, Hongsermeier C, Trivedi V, Jovan J, Nussinov Z, Seidel A, Li F, Shen M, Leu W, Hite H, Dunn J, Buras W, Gao J, Sumer B, Akers WJ, Achilefu S IEEE Transactions on Biomedical Engineering 2026 -
Targeting severe acidity for tumor-activatable Interleukin-2 therapy
Feng Q, Pantoja R, Lopez JG, Li W, Sun Z, Wang Q, Ye S, Basava VS, Huang G, Torres K, Chen M, Yue T, Sumer BD, Gao J Cell Reports Medicine 2026 Jan 7 -
Protocol for integrating immunohistochemistry and H&E annotations with Xenium data at single-cell resolution
Chen J, Hartnett W, Basava VS, Lee M, Sumer BD, Gao J, Feng Q STAR Protocols 2025 Dec 6 -
HYHOPE: A Phase 1 Study of Deintensified Hypofractionated Radiation Therapy for Human Papillomavirus-Associated Oropharynx Cancer
Moon DH, Avkshtol V, Hughes RS, Ahn C, Sumer BD, Day AT, Tillman BN, Myers LL, Truelson JM, Sher DJ International Journal of Radiation Oncology Biology Physics 2025 Nov 123 694-702 -
Stimuli-responsive STING nanovaccine for systemic therapy of HPV-induced cancers
Chen S, Ye S, Huang G, Sun Z, Feng Q, Wang M, Pantoja R, Sumer BD, Gao J Proceedings of the National Academy of Sciences of the United States of America 2025 Nov 122 -
Relationship Between Elective Neck Irradiation and Severe Lymphopenia in Patients Treated With Head and Neck Chemoradiotherapy
Mickel TA, Moon DH, Avkshtol V, Pham NL, Shah JL, Hughes RS, Sumer BD, Sher DJ Clinical Oncology 2025 Aug 44 -
Margin Status and Recurrence in Surgically Treated Patients With HPV+ Oropharyngeal Cancer
Ausburn M, Pyne JM, Day AT, Hajnas N, Moon D, Myers LL, Sher DJ, Truelson JM, Tillman B, Sumer B Laryngoscope 2025 Aug 135 2777-2782 -
A Multi-Threshold Micelle Improves Tumor Accumulation and STING Immunotherapy
Bennett ZT, Krishnamurthy A, Ye S, Basava VS, Feng Q, Huang G, Sumer BD, Gao J Journal of the American Chemical Society 2025 Jun 147 19547-19558 -
Nodal Yield From Neck Dissection Predicts the Anti-Tumor Immune Response in Head and Neck Cancers
Chen S, Pyne JM, Liu Y, Abraham Y, Wen Z, Palsgrove D, Xiao G, Truelson J, Myers L, Tillman B, Day A, Gordin E, Stankova L, Xie Y, Sher D, Bishop J, Gao J, Sumer BD Head and Neck 2025 Apr 47 1199-1208 -
Stereotactic Ablative Radiotherapy for T1 to T2 Glottic Larynx Cancer: Mature Results From the Phase 2 GLoTtic Larynx-SABR Trial
Sher DJ, Avkshtol V, Moon D, Vo D, Mau T, Childs L, Lin MH, Dubas J, Ahn C, Sumer BD International Journal of Radiation Oncology Biology Physics 2025 Jan 121 137-144 -
Fluorescence-Guided Surgery for Assessing Margins in Head and Neck Cancer A Review
Gowrishankar S, Van Keulen S, Mattingly A, Tanaka H, Topf M, Mannion K, Langerman A, Rohde S, Sinard R, Choe J, Sumer B, Varvares M, Rosenthal EL JAMA Surgery 2025 -
Stepwise Ultra-pH-Sensitive Micelles Overcome a pKa Barrier for Systemic Lymph Node Delivery
Bennett ZT, Huang G, Dellinger MT, Sumer BD, Gao J ACS Nano 2024 Jul 18 16632-16647 -
Severely polarized extracellular acidity around tumour cells
Feng Q, Bennett Z, Grichuk A, Pantoja R, Huang T, Faubert B, Huang G, Chen M, DeBerardinis RJ, Sumer BD, Gao J Nature Biomedical Engineering 2024 Jun 8 787-799 -
STING licensing of type I dendritic cells potentiates antitumor immunity
Wang J, Li S, Wang M, Wang X, Chen S, Sun Z, Ren X, Huang G, Sumer BD, Yan N, Fu YX, Gao J Science Immunology 2024 Feb 9 -
International Consensus Statement on Allergy and Rhinology: Sinonasal Tumors
Kuan EC, Wang EW, Adappa ND, Beswick DM, London NR, Su SY, Wang MB, Abuzeid WM, Alexiev B, Alt JA, Antognoni P, Alonso-Basanta M, Batra PS, Bhayani M, Bell D, Bernal-Sprekelsen M, Betz CS, Blay JY, Bleier BS, Bonilla-Velez J, Callejas C, Carrau RL, Casiano RR, Castelnuovo P, Chandra RK, Chatzinakis V, Chen SB, Chiu AG, Choby G, Chowdhury NI, Citardi MJ, Cohen MA, Dagan R, Dalfino G, Dallan I, Dassi CS, de Almeida J, Dei Tos AP, DelGaudio JM, Ebert CS, El-Sayed IH, Eloy JA, Evans JJ, Fang CH, Farrell NF, Ferrari M, Fischbein N, Folbe A, Fokkens WJ, Fox MG, Lund VJ, Gallia GL, Gardner PA, Geltzeiler M, Georgalas C, Getz AE, Govindaraj S, Gray ST, Grayson JW, Gross BA, Grube JG, Guo R, Ha PK, Halderman AA, Hanna EY, Harvey RJ, Hernandez SC, Holtzman AL, Hopkins C, Huang Z, Huang Z, Humphreys IM, Hwang PH, Iloreta AM, Ishii M, Ivan ME, Jafari A, Kennedy DW, Khan M, Kimple AJ, Kingdom TT, Knisely A, Kuo YJ, Lal D, Lamarre ED, Lan MY, Le H, Lechner M, Lee NY, Lee JK, Lee VH, Levine CG, Lin JC, Lin DT, Lobo BC, Locke T, Luong AU, Magliocca KR, Markovic SN, Matnjani G, McKean EL, Meço C, Mendenhall WM, Michel L, Na'ara S, Nicolai P, Nuss DW, Nyquist GG, Oakley GM, Omura K, Orlandi RR, Otori N, Papagiannopoulos P, Patel ZM, Pfister DG, Phan J, Psaltis AJ, Rabinowitz MR, Ramanathan M, Rimmer R, Rosen MR, Sanusi O, Sargi ZB, Schafhausen P, Schlosser RJ, Sedaghat AR, Senior BA, Shrivastava R, Sindwani R, Smith TL, Smith KA, Snyderman CH, Solares CA, Sreenath SB, Stamm A, Stölzel K, Sumer B, Surda P, Tajudeen BA, Thompson LD, Thorp BD, Tong CC, Tsang RK, Turner JH, Turri-Zanoni M, Udager AM, van Zele T, VanKoevering K, Welch KC, Wise SK, Witterick IJ, Won TB, Wong SN, Woodworth BA, Wormald PJ, Yao WC, Yeh CF, Zhou B, Palmer JN International Forum of Allergy and Rhinology 2024 Feb 14 149-608 -
Comparison of da Vinci Single Port vs Si Systems for Transoral Robotic-Assisted Surgery A Review With Technical Insights
Oberhelman N, Bruening J, Jackson RS, Van Abel KM, Sumer B, Holsinger FC, Chan JY, Gross ND, Clayburgh DR, Andersen PE, Li RJ JAMA Otolaryngology - Head and Neck Surgery 2024 Feb 150 165-171 -
An Ensemble Learning Method for Detection of Head and Neck Squamous Cell Carcinoma Using Polarized Hyperspectral Microscopic Imaging
Mubarak HK, Zhou X, Palsgrove D, Sumer BD, Chen AY, Fei B 2024 -
Polarized hyperspectral microscopic imaging system for enhancing the visualization of collagen fibers and head and neck squamous cell carcinoma
Zhou X, Ma L, Mubarak HK, Palsgrove D, Sumer BD, Chen AY, Fei B Journal of biomedical optics 2024 Jan 29 -
HYPORT: Phase 1 Study of 3-Week Hypofractionated Postoperative Radiation Therapy for Head and Neck Squamous Cell Carcinoma
Moon DH, Avkshtol V, Vo D, Ahn C, Sumer B, Day AT, Tillman B, Myers L, Truelson J, Sher DJ International Journal of Radiation Oncology Biology Physics 2024 Jan 118 157-164 -
Efficacy and Quality-of-Life Following Involved Nodal Radiotherapy for Head and Neck Squamous Cell Carcinoma: The INRT-AIR Phase II Clinical Trial
Sher DJ, Moon DH, Vo D, Wang J, Chen L, Dohopolski M, Hughes R, Sumer BD, Ahn C, Avkshtol V Clinical Cancer Research 2023 Sep 29 3284-3291 -
Long-term Patient-Reported Outcomes in a Population-Based Cohort Following Radiotherapy vs Surgery for Oropharyngeal Cancer
Dohopolski MJ, Diao K, Hutcheson KA, Akhave NS, Goepfert RP, He W, Lei XJ, Peterson SK, Shen Y, Sumer BD, Smith BD, Sher DJ JAMA Otolaryngology - Head and Neck Surgery 2023 Aug 149 697-707 -
Adherence to the American Cancer Society Head and Neck Cancer Survivorship Care Guideline According to Chart Review: A Nested Retrospective Cohort Pilot Study
Salley JR, Day AT, Balachandra S, Mehr J, Sumer BD, Sher DJ, Mayfield Arnold E, Danphuong Ho E, Lee SC, Eary R Annals of Otology, Rhinology and Laryngology 2023 May 132 481-491 -
Intraoperative molecular imaging: 3rd biennial clinical trials update
Bou-Samra P, Muhammad N, Chang A, Karsalia R, Azari F, Kennedy G, Stummer W, Tanyi J, Martin L, Vahrmeijer A, Smith B, Rosenthal E, Wagner P, Rice D, Lee A, Abdelhafeez A, Malek MM, Kohanbash G, Barry Edwards W, Henderson E, Skjøth-Rasmussen J, Orosco R, Gibbs S, Farnam RW, Shankar L, Sumer B, Kumar AT, Marcu L, Li L, Greuv V, Delikatny EJ, Lee JY, Singhal S Journal of biomedical optics 2023 May 28 -
Patient-Reported Financial Toxicity in a Population-Based Cohort of Oropharynx Cancer Survivors
Diao K, Lei X, Smith GL, Jagsi R, Peterson SE, Sumer BD, Smith BD, Sher DJ International Journal of Radiation Oncology Biology Physics 2023 May 116 142-153 -
Polarized hyperspectral microscopic imaging for collagen visualization on pathologic slides of head and neck squamous cell carcinoma
Zhou X, Mubarak HK, Ma L, Palsgrove D, Sumer BD, Fei B 2023 -
Lactate increases stemness of CD8 + T cells to augment anti-tumor immunity
Feng Q, Liu Z, Yu X, Huang T, Chen J, Wang J, Wilhelm J, Li S, Song J, Li W, Sun Z, Sumer BD, Li B, Fu YX, Gao J Nature communications 2022 Dec 13 -
Characteristics and outcomes of young patients with laryngeal cancer: National hospital-based retrospective cohort analysis
Yang A, Tanamal P, Tibbetts K, Sumer B, Blackwell JM, Schostag K, Sher D, Day A Head and Neck 2022 Oct 44 2095-2108 -
Clinical and Biologic Characteristics and Outcomes in Young and Middle-Aged Patients With Laryngeal Cancer: A Retrospective Cohort Analysis
Geng CX, Tanamal P, Arvisais-Anhalt S, Tomasino M, Gheit T, Bishop JA, Palsgrove DN, Wang E, Salley JR, Tibbetts K, Sumer BD, Tillman BN, Day AT Otolaryngology - Head and Neck Surgery (United States) 2022 Oct 167 688-698 -
Long-term opioid use in patients treated with head and neck intensity-modulated radiotherapy
Zhao L, Moon DH, Avkshtol V, Siropaides CH, Terauchi S, Day AT, Sumer BD, Hughes R, Sher DJ Supportive Care in Cancer 2022 Sep 30 7517-7525 -
Smoking and other patient factors in HPV-mediated oropharynx cancer: A retrospective cohort study
Schostag K, Lynch PT, Leavitt T, Sumer BD, Yang A, Shah A, Emmet TR, Sher DJ, Day AT American Journal of Otolaryngology - Head and Neck Medicine and Surgery 2022 Sep 43 -
Survival and disease progression following solitary locoregional recurrence after head and neck radiotherapy
Zhao L, Day AT, Moon D, Avkshtol V, Sumer BD, Hughes R, Sher DJ Head and Neck 2022 May 44 1153-1163 -
Intratumoral administration of STING-activating nanovaccine enhances T cell immunotherapy
Jiang X, Wang J, Zheng X, Liu Z, Zhang X, Li Y, Wilhelm J, Cao J, Huang G, Zhang J, Sumer B, Lea J, Lu Z, Gao J, Luo M Journal for ImmunoTherapy of Cancer 2022 May 10 -
Erratum: Automatic detection of head and neck squamous cell carcinoma on histologic slides using hyperspectral microscopic imaging (J. Biomed. Opt. (2022) 27:4 (046501) DOI: 10.1117/1.JBO.27.4.046501)
Ma L, Little JV, Chen AY, Myers L, Sumer BD, Fei B Journal of biomedical optics 2022 May 27 -
Automatic detection of head and neck squamous cell carcinoma on histologic slides using hyperspectral microscopic imaging
Ma L, Little JV, Chen AY, Myers L, Sumer BD, Fei B Journal of biomedical optics 2022 Apr 27 -
Pilot Study of a Wearable Activity Monitor during Head and Neck Radiotherapy to Predict Clinical Outcomes
Sher DJ, Radpour S, Shah JL, Pham NL, Jiang S, Vo D, Sumer BD, Day AT JCO Clinical Cancer Informatics 2022 6 -
Substance use and mental health burden in head and neck and other cancer survivors: A National Health Interview Survey analysis
Balachandra S, Eary RL, Lee R, Wynings EM, Sher DJ, Sura T, Liu Y, Tillman BN, Sumer BD, Arnold EM, Tiro JA, Lee SC, Day AT Cancer 2022 Jan 128 112-121 -
Automatic detection of head and neck squamous cell carcinoma on pathologic slides using polarized hyperspectral imaging and deep learning
Zhou X, Ma L, Mubarak HK, Little JV, Chen AY, Myers LL, Sumer BD, Fei B 2022 -
A Standardized Framework for Fluorescence-Guided Margin Assessment for Head and Neck Cancer Using a Tumor Acidosis Sensitive Optical Imaging Agent
Steinkamp PJ, Voskuil FJ, van der Vegt B, Doff JJ, Schepman KP, de Visscher SA, Kelder W, Jayalakshmi Y, Gao J, Sumer BD, van Dam GM, Witjes MJ Molecular Imaging and Biology 2021 Dec 23 809-817 -
Prognostic impact of matted lymphadenopathy in patients with oropharyngeal squamous cell carcinoma treated with definitive chemoradiotherapy
Burningham K, Moore W, Moon D, Avkshtol V, Day AT, Sumer B, Vo D, Bishop JA, Hughes R, Sher DJ Oral Oncology 2021 Dec 123 -
Effect of COVID-19 pandemic lockdowns on planned cancer surgery for 15 tumour types in 61 countries: an international, prospective, cohort study
Author Collaboration CC, Glasbey JC, Ademuyiwa A, Adisa A, AlAmeer E, Arnaud AP, Ayasra F, Azevedo J, Bravo AM, Costas-Chavarri A, Edwards J, Elhadi M, Fiore M, Fotopoulou C, Gallo G, Ghosh D, Griffiths EA, Harrison E, Hutchinson P, Lawani I, Lawday S, Lederhuber H, Leventoglu S, Li E, Gomes GM, Mann H, Marson EJ, Martin J, Mazingi D, McLean K, Modolo M, Moore R, Morton D, Ntirenganya F, Pata F, Picciochi M, Pockney P, Ramos-De La Medina A, Roberts K, Roslani AC, Seenivasagam RK, Shaw R, Simões JF, Smart N, Stewart GD, Sullivan R, Sundar S, Williams N, Aoun SG, Batjer HH, Sumer B The Lancet Oncology 2021 Nov 22 1507-1517 -
The Changing Demographics and Treatment of Larynx Cancer
Han J, Sumer BD Annals of Surgical Oncology 2021 Nov 28 6927-6928 -
Institutional patterns of head and neck oncology care during the early phase of the COVID-19 pandemic: A retrospective, pooled cross-sectional analysis
Shah A, Sumer BD, Schostag K, Balachandra S, Sher DJ, Gordin EA, Day AT Oral Oncology 2021 Nov 122 -
Extracapsular extension, pathologic node status, and adjuvant treatment in primary surgery patients with human papillomavirus-mediated oropharyngeal cancer: National hospital-based retrospective cohort analysis
Day AT, Yang AM, Tanamal P, Blackwell JM, Wang E, Sumer BD, Bishop JA, Hughes RS, Khan S, Sher DJ Head and Neck 2021 Nov 43 3345-3363 -
Global wealth disparities drive adherence to COVID-safe pathways in head and neck cancer surgery
Author Collaboration CC, Schache AG, Shaw R, Winter SC, Glasbey J, Ganly I, Batstone M, Biel JR, Simon C, Omar O, Simoes JF, Nepogodiev D, Bhangu A, Pinkney T, McGill L, Perry R, Hughes T, Jackson R, Glasbey JC, Ho MW, Abbott TE, Adamina M, Ademuyiwa AO, Agarwal A, Alameer E, Alderson D, Alakaloko F, Albertsmeiers M, Alser O, Alshaar M, Alshryda S, Arnaud AP, Augestad KM, Ayasra F, Azevedo J, Bankhead-Kendall BK, Barlow E, Benson RA, Colino RB, Brar A, Minaya-Bravo A, Breen KA, Bretherton C, Buarque IL, Burke J, Caruana EJ, Chaar M, Chakrabortee S, Christensen P, Cox D, Sumer B BJS open 2021 Nov 5 -
Polyvalent design in the cGAS-STING pathway
Bennett ZT, Li S, Sumer BD, Gao J Seminars in Immunology 2021 Aug 56 -
Factors Associated with Lymph Node Count in Mucosal Squamous Cell Carcinoma Neck Dissection
Bhalli H, Chen S, Day A, Tillman B, Gordin E, Truelson J, Sher D, Myers L, Gao J, Sumer BD Laryngoscope 2021 Jul 131 1516-1521 -
Editorial: Cancer Staging in Squamous Cell Carcinoma of the Vermilion Lip
Sumer BD Annals of Surgical Oncology 2021 Jun 28 2944-2945 -
Effectiveness of physical activity interventions in improving objective and patient-reported outcomes in head and neck cancer survivors: A systematic review
Lynch PT, Horani S, Lee R, Sumer BD, Lee SC, Mayo HG, Rethorst CD, Day AT Oral Oncology 2021 Jun 117 -
Intraoperative molecular imaging clinical trials: A review of 2020 conference proceedings
Azari F, Kennedy G, Bernstein E, Hadjipanayis C, Vahrmeijer AL, Smith BL, Rosenthal E, Sumer B, Tian J, Henderson ER, Lee A, Nguyen Q, Gibbs SL, Pogue BW, Orringer DA, Charalampaki P, Martin LW, Tanyi JL, Kenneth Lee M, Lee JY, Singhal S Journal of biomedical optics 2021 May 26 -
Author Correction: Prolonged activation of innate immune pathways by a polyvalent STING agonist (Nature Biomedical Engineering, (2021), 5, 5, (455-466), 10.1038/s41551-020-00675-9)
Li S, Luo M, Wang Z, Feng Q, Wilhelm J, Wang X, Li W, Wang J, Cholka A, Fu Yx, Sumer BD, Yu H, Gao J Nature Biomedical Engineering 2021 May 5 483 -
Prolonged activation of innate immune pathways by a polyvalent STING agonist
Li S, Luo M, Wang Z, Feng Q, Wilhelm J, Wang X, Li W, Wang J, Cholka A, Fu Yx, Sumer BD, Yu H, Gao J Nature Biomedical Engineering 2021 May 5 455-466 -
Blood-based biomarkers of human papillomavirus–associated cancers: A systematic review and meta-analysis
Balachandra S, Kusin SB, Lee R, Blackwell JM, Tiro JA, Cowell LG, Chiang CM, Wu SY, Varma S, Rivera EL, Mayo HG, Ding L, Sumer BD, Lea JS, Bagrodia A, Farkas LM, Wang R, Fakhry C, Dahlstrom KR, Sturgis EM, Day AT Cancer 2021 Mar 127 850-864 -
Editorial Comment on “Enhanced Recovery After Surgery (ERAS) in Head and Neck Oncologic Surgery: A Case-Matched Analysis of Perioperative and Pain Outcomes”
Chen S, Sumer BD Annals of Surgical Oncology 2021 Feb 28 604-605 -
Tumor-Targeted Inhibition of Monocarboxylate Transporter 1 Improves T-Cell Immunotherapy of Solid Tumors
Huang T, Feng Q, Wang Z, Li W, Sun Z, Wilhelm J, Huang G, Vo T, Sumer BD, Gao J Advanced Healthcare Materials 2021 Feb 10 -
Hyperspectral microscopic imaging for the detection of head and neck squamous cell carcinoma on histologic slides
Ma L, Zhou X, Little JV, Chen AY, Myers LL, Sumer BD, Fei B 2021 -
Pixel-level tumor margin assessment of surgical specimen with hyperspectral imaging and deep learning classification
Ma L, Shahedi M, Shi T, Halicek M, Little JV, Chen AY, Myers LL, Sumer BD, Fei B 2021 -
Automatic detection of head and neck squamous cell carcinoma on pathologic slides using polarized hyperspectral imaging and machine learning
Zhou X, Ma L, Brown W, Little JV, Chen AY, Myers LL, Sumer BD, Fei B 2021 -
Exploiting metabolic acidosis in solid cancers using a tumor-agnostic pH-activatable nanoprobe for fluorescence-guided surgery
Author Collaboration tS, Voskuil FJ, Steinkamp PJ, Zhao T, van der Vegt B, Koller M, Doff JJ, Jayalakshmi Y, Hartung JP, Gao J, Sumer BD, Witjes MJ, van Dam GM, Albaroodi Y, Been LB, Dijkstra F, van Etten B, Feng Q, van Ginkel RJ, Hall K, Havenga K, Haveman JW, Hemmer PH, Jansen L, de Jongh SJ, Kats-Ugurlu G, Kelder W, Kruijff S, Kruithof I, van Loo E, Roodenburg JL, Shenoy N, Schepman KP, de Visscher SA Nature communications 2020 Dec 11 -
Nano-Immune-Engineering Approaches to Advance Cancer Immunotherapy: Lessons from Ultra-pH-Sensitive Nanoparticles
Li S, Bennett ZT, Sumer BD, Gao J Accounts of Chemical Research 2020 Nov 53 2546-2557 -
COVID-19 Pandemic and Surgical Oncology: Preserving the Academic Mission
Pawlik TM, Tyler DS, Sumer B, Meric-Bernstam F, Okereke IC, Beane JD, Dedhia PH, Ejaz A, McMasters KM, Tanabe KK Annals of Surgical Oncology 2020 Aug 27 2591-2599 -
Head and neck oncology during the COVID-19 pandemic: Reconsidering traditional treatment paradigms in light of new surgical and other multilevel risks
Day AT, Sher DJ, Lee RC, Truelson JM, Myers LL, Sumer BD, Stankova L, Tillman BN, Hughes RS, Khan SA, Gordin EA Oral Oncology 2020 Jun 105 -
PET imaging of occult tumours by temporal integration of tumour-acidosis signals from pH-sensitive 64Cu-labelled polymers
Huang G, Zhao T, Wang C, Nham K, Xiong Y, Gao X, Wang Y, Hao G, Ge WP, Sun X, Sumer BD, Gao J Nature Biomedical Engineering 2020 Mar 4 314-324 -
Unique Patterns of Distant Metastases in HPV-Positive Head and Neck Cancer
Sacks R, Law JY, Zhu H, Beg MS, Gerber DE, Sumer BD, Myers LL, Truelson JM, Nedzi L, Sher D, Hughes RS, Khan SA Oncology (Switzerland) 2020 Feb 98 179-185 -
Detection of lymph node metastases by ultra-pH-sensitive polymeric nanoparticles
Bennett ZT, Feng Q, Bishop JA, Huang G, Sumer BD, Gao J Theranostics 2020 10 3340-3350 -
Neck Dissection and Parotidectomy for Melanoma
Gastman B, Knackstedt R, Goepfert RP, Sumer B, Shaha A, Kupferman ME 2020 Jan 1 689-704 -
In Reply to Mendenhall et al
Sher DJ, Timmerman RD, Nedzi LA, Ding C, Pham NL, Zhao B, Sumer BD International Journal of Radiation Oncology Biology Physics 2020 Jan 106 221 -
Exploiting nanoscale cooperativity for precision medicine
Wilhelm J, Wang Z, Sumer BD, Gao J Advanced Drug Delivery Reviews 2020 Jan 158 63-72 -
Translational Research: Bridging the Gap between Fundamental Research and the Clinic
Dai Z, Man NK, Parak WJ, Smith B, Sumer BD, Tang BZ, Van Hest J, Rotello VM Bioconjugate Chemistry 2019 Dec 30 2989-2990 -
Head and Neck Cancer Detection in Digitized Whole-Slide Histology Using Convolutional Neural Networks
Halicek M, Shahedi M, Little JV, Chen AY, Myers LL, Sumer BD, Fei B Scientific reports 2019 Dec 9 -
Head and neck neuroendocrine tumors at a single institution over 15 years
Bacalao M, Beg MS, Cavuoti D, Zhu H, Sumer B, Myers L, Truelson J, Nedzi L, Sher D, Hughes R, Khan SA Clinical Case Reports 2019 Dec 7 2508-2512 -
Phase 1 Fractional Dose-Escalation Study of Equipotent Stereotactic Radiation Therapy Regimens for Early-Stage Glottic Larynx Cancer
Sher DJ, Timmerman RD, Nedzi L, Ding C, Pham NL, Zhao B, Sumer BD International Journal of Radiation Oncology Biology Physics 2019 Sep 105 110-118 -
Hyperspectral imaging of head and neck squamous cell carcinoma for cancer margin detection in surgical specimens from 102 patients using deep learning
Halicek M, Dormer JD, Little JV, Chen AY, Myers L, Sumer BD, Fei B Cancers 2019 Sep 11 -
Hyperspectral imaging for head and neck cancer detection: Specular glare and variance of the tumor margin in surgical specimens
Halicek M, Fabelo H, Ortega S, Little JV, Wang X, Chen AY, Callico GM, Myers L, Sumer BD, Fei B Journal of Medical Imaging 2019 Jul 6 -
Synergistic STING activation by PC7A nanovaccine and ionizing radiation improves cancer immunotherapy
Luo M, Liu Z, Zhang X, Han C, Samandi LZ, Dong C, Sumer BD, Lea J, Fu YX, Gao J Journal of Controlled Release 2019 Apr 300 154-160 -
Risk of Unplanned Hospital Encounters in Patients Treated With Radiotherapy for Head and Neck Squamous Cell Carcinoma
Moore ZR, Pham NL, Shah JL, Nedzi L, Sumer BD, Day AT, Khan SA, Sher DJ Journal of Pain and Symptom Management 2019 Apr 57 738-745.e3 -
Association between treatment delays and oncologic outcome in patients treated with surgery and radiotherapy for head and neck cancer
Tumati V, Hoang L, Sumer BD, Truelson JM, Myers LL, Khan S, Hughes RS, Nedzi LA, Sher DJ Head and Neck 2019 Feb 41 315-321 -
Detection of squamous cell carcinoma in digitized histological images from the head and neck using convolutional neural networks
Halicek M, Shahedi M, Little JV, Chen AY, Myers LL, Sumer BD, Fei B 2019 -
Salvage laryngectomy and laryngopharyngectomy: Multicenter review of outcomes associated with a reconstructive approach
Author Collaboration MC, Oxford LE, Urken M, Lazarus C, Cheney J, Scharpf J, Fritz MA, Puscas L, Mlynarek AM, Sela E, Ibrahim B, Hier MP, Hanasono MM, Yu P, Hornig JD, Miles B, Teng M, Genden E, Patel UA, Lin AC, Malone JP, Rosenthal EL, Clemons L, Zhang H, O'Connell DA, Ansari K, Harris JR, Seikaly H, Moreno MA, Luu Q, Jacobson J, Farwell DG, Blackwell K, Zaghi S, Nabili V, Wang SJ, Burgess BC, Casper K, Goddard J, Bayon R, Pagedar NA, Chang KE, Hoffman HT, Shnayder Y, Bond J, Sykes KJ, Girod DA, Tsue TT, Myers LL, Sumer BD, Truelson JM Head and Neck 2019 Jan 41 16-29 -
Cancer detection using hyperspectral imaging and evaluation of the superficial tumor margin variance with depth
Halicek M, Fabelo H, Ortega S, Little JV, Wang X, Chen AY, Callico GM, Myers LL, Sumer BD, Fei B 2019 -
Targeting NAD + Metabolism to Enhance Radiation Therapy Responses
Lewis JE, Singh N, Holmila RJ, Sumer BD, Williams NS, Furdui CM, Kemp ML, Boothman DA Seminars in Radiation Oncology 2019 Jan 29 6-15 -
Comparative effectiveness of primary radiotherapy versus surgery in elderly patients with locally advanced oropharyngeal squamous cell carcinoma
Sher DJ, Yan J, Day A, Sumer BD, Pham NL, Khan S, Zhu H Oral Oncology 2019 Jan 88 18-26 -
Final results of a multi-institutional phase II trial of reirradiation with concurrent weekly cisplatin and cetuximab for recurrent or second primary squamous cell carcinoma of the head and neck
Awan MJ, Nedzi L, Wang D, Tumati V, Sumer B, Xie XJ, Smith I, Truelson J, Hughes R, Myers LL, Lavertu P, Wong S, Yao M Annals of Oncology 2018 Apr 29 998-1003 -
Optical molecular imaging for tumor detection and image-guided surgery
Wang C, Wang Z, Zhao T, Li Y, Huang G, Sumer BD, Gao J Biomaterials 2018 Mar 157 62-75 -
Risk of contralateral nodal failure following ipsilateral IMRT for node-positive tonsillar cancer
Gottumukkala S, Pham NL, Sumer B, Myers L, Truelson J, Nedzi L, Khan S, Hughes R, Sher DJ Oral Oncology 2017 Dec 75 35-38 -
Treatment Deintensification for Human Papillomavirus-Associated Oropharyngeal Cancer
Arnaoutakis D, Sumer BD Annals of Surgical Oncology 2017 Nov 24 3463-3465 -
Clinical practice in PET/CT for the management of head and neck squamous cell cancer
Goel R, Moore W, Sumer B, Khan S, Sher D, Subramaniam RM American Journal of Roentgenology 2017 Aug 209 289-303 -
Model to Predict Cause-Specific Mortality in Patients with Head and Neck Adenoid Cystic Carcinoma: A Competing Risk Analysis
Imanguli M, Sumer BD Annals of Surgical Oncology 2017 Aug 24 2069-2070 -
Improving patient health engagement with mobile texting: A pilot study in the head and neck postoperative setting
Sosa A, Heineman N, Thomas K, Tang K, Feinstein M, Martin MY, Sumer B, Schwartz DL Head and Neck 2017 May 39 988-995 -
SBRT for early-stage glottic larynx cancer-Initial clinical outcomes from a phase i clinical trial
Schwartz DL, Sosa A, Chun SG, Ding C, Xie XJ, Nedzi LA, Timmerman RD, Sumer BD PloS one 2017 Mar 12 -
Phantom-to-clinic development of hypofractionated stereotactic body radiotherapy for early-stage glottic laryngeal cancer
Ding C, Chun SG, Sumer BD, Nedzi LA, Abdulrahman RE, Yordy JS, Lee P, Hrycushko B, Solberg TD, Ahn C, Timmerman RD, Schwartz DL Medical Dosimetry 2017 Feb 42 90-96 -
A transistor-like pH nanoprobe for tumour detection and image-guided surgery
Zhao T, Huang G, Li Y, Yang S, Ramezani S, Lin Z, Wang Y, Ma X, Zeng Z, Luo M, De Boer E, Xie XJ, Thibodeaux J, Brekken RA, Sun X, Sumer BD, Gao J Nature Biomedical Engineering 2017 Jan 1 -
Online dosimetric evaluation of larynx SBRT: A pilot study to assess the necessity of adaptive replanning
Mao W, Rozario T, Lu W, Gu X, Yan Y, Jia X, Sumer B, Schwartz DL Journal of applied clinical medical physics 2017 18 157-163 -
A Phase I/II Study of Nab-Paclitaxel, Cisplatin, and Cetuximab With Concurrent Radiation Therapy for Locally Advanced Squamous Cell Cancer of the Head and Neck
Chun SG, Hughes R, Sumer BD, Myers LL, Truelson JM, Khan SA, Ma TW, Xie Y, Yordy JS, Cooley S, Wu J, Choy H, Nedzi LA Cancer Investigation 2017 Jan 35 23-31 -
Digitization of Endocytic pH by Hybrid Ultra-pH-Sensitive Nanoprobes at Single-Organelle Resolution
Wang Y, Wang C, Li Y, Huang G, Zhao T, Ma X, Wang Z, Sumer BD, White MA, Gao J Advanced Materials 2017 Jan 29 -
Erratum: Molecular basis of cooperativity in pH-triggered supramolecular self-assembly (Nature Communications, (2016), 7, 1, (13214), 10.1038/ncomms13214)
Li Y, Zhao T, Wang C, Lin Z, Huang G, Sumer BD, Gao J Nature communications 2016 Dec 7 -
Non-covalent interactions in controlling pH-responsive behaviors of self-assembled nanosystems
Li Y, Wang Z, Wei Q, Luo M, Huang G, Sumer BD, Gao J Polymer Chemistry 2016 Oct 7 5949-5956 -
Molecular basis of cooperativity in pH-triggered supramolecular self-assembly
Li Y, Zhao T, Wang C, Lin Z, Huang G, Sumer BD, Gao J Nature communications 2016 Oct 7 -
Patterns of care and comparative effectiveness of intensified adjuvant therapy for resected oropharyngeal squamous cell carcinoma in the human papillomavirus era
Sher DJ, Nedzi L, Khan S, Hughes R, Sumer BD, Myers LL, Truelson JM, Koshy M JAMA Otolaryngology - Head and Neck Surgery 2016 Aug 142 777-788 -
NQO1-Mediated tumor-selective lethality and radiosensitization for head and neck cancer
Li LS, Reddy S, Lin ZH, Liu S, Park H, Chun SG, Bornmann WG, Thibodeaux J, Yan J, Chakrabarti G, Xie XJ, Sumer BD, Boothman DA, Yordy JS Molecular Cancer Therapeutics 2016 Jul 15 1757-1767 -
Successful translation of fluorescence navigation during oncologic surgery: A consensus report
Rosenthal EL, Warram JM, De Boer E, Basilion JP, Biel MA, Bogyo M, Bouvet M, Brigman BE, Colson YL, DeMeester SR, Gurtner GC, Ishizawa T, Jacobs PM, Keereweer S, Liao JC, Nguyen QT, Olson JM, Paulsen KD, Rieves D, Sumer BD, Tweedle MF, Vahrmeijer AL, Weichert JP, Wilson BC, Zenn MR, Zinn KR, Van Dam GM Journal of Nuclear Medicine 2016 Jan 57 144-150 -
En Bloc Resection of the Temporal Bone and Temporomandibular Joint for Advanced Temporal Bone Carcinoma
Kutz JW, Mitchell D, Isaacson B, Roland PS, Allen KP, Sumer BD, Barnett S, Truelson JM, Myers LL Otolaryngology-Head and Neck Surgery 2015 Mar 152 571-573 -
Ultra-pH-sensitive nanoprobe library with broad pH tunability and fluorescence emissions
Ma X, Wang Y, Zhao T, Li Y, Su LC, Wang Z, Huang G, Sumer BD, Gao J Journal of the American Chemical Society 2014 Aug 136 11085-11092 -
In vivo optical imaging of folate receptor-β in head and neck squamous cell carcinoma
Sun JY, Shen J, Thibodeaux J, Huang G, Wang Y, Gao J, Low PS, Dimitrov DS, Sumer BD Laryngoscope 2014 Aug 124 E312-E319 -
A nanoparticle-based strategy for the imaging of a broad range of tumours by nonlinear amplification of microenvironment signals
Wang Y, Zhou K, Huang G, Hensley C, Huang X, Ma X, Zhao T, Sumer BD, Deberardinis RJ, Gao J Nature Materials 2014 Feb 13 204-212 -
Transoral robotic surgery and transoral laser microsurgery for oropharyngeal squamous cell cancer
Sumer BD, Goyal V, Truelson JM, Myers LL Journal of Robotic Surgery 2013 Dec 7 377-383 -
Transoral robotic surgery: Simulation-based standardized training
Zhang N, Sumer BD JAMA Otolaryngology - Head and Neck Surgery 2013 Nov 139 1111-1117 -
Multi-chromatic pH-activatable 19F-MRI nanoprobes with binary ON/OFF pH transitions and chemical-shift barcodes
Huang X, Huang G, Zhang S, Sagiyama K, Togao O, Ma X, Wang Y, Li Y, Soesbe TC, Sumer BD, Takahashi M, Sherry AD, Gao J Angewandte Chemie - International Edition 2013 Jul 52 8074-8078 -
Surgery for carcinoma of the oral cavity
Crozier E, Sumer BD Otorinolaringologia 2012 Sep 62 141-147 -
Multicolored pH-tunable and activatable fluorescence nanoplatform responsive to physiologic pH stimuli
Zhou K, Liu H, Zhang S, Huang X, Wang Y, Huang G, Sumer BD, Gao J Journal of the American Chemical Society 2012 May 134 7803-7811 -
Theranostic Polymeric Micelles for Cancer Imaging and Therapy
Huang G, Khemtong C, Bey EA, Boothman DA, Sumer BD, Gao J 2012 257-276 -
Photoactivation switch from type II to type i reactions by electron-rich micelles for improved photodynamic therapy of cancer cells under hypoxia
Ding H, Yu H, Dong Y, Tian R, Huang G, Boothman DA, Sumer BD, Gao J Journal of Controlled Release 2011 Dec 156 276-280 -
Impact of treatment sequence of multimodal therapy for advanced oral cavity cancer with mandible invasion
Myers LL, Sumer BD, Truelson JM, Nedzi L, Perkins S, Hughes RS, Ahn C Otolaryngology - Head and Neck Surgery 2011 Dec 145 961-966 -
Overcoming endosomal barrier by amphotericin B-loaded dual pH-responsive PDMA- b-PDPA micelleplexes for siRNA delivery
Yu H, Zou Y, Wang Y, Huang X, Huang G, Sumer BD, Boothman DA, Gao J ACS Nano 2011 Nov 5 9246-9255 -
Characterization and optimization of mTHPP nanoparticles for photodynamic therapy of head and neck cancer
Ding H, Mora R, Gao J, Sumer BD Otolaryngology - Head and Neck Surgery 2011 Oct 145 612-617 -
Resection and free tissue reconstruction of locally advanced oral cancer: Avoidance of lip split
Myers LL, Sumer BD, Truelson JM, Ahn C, Leach JL Microsurgery 2011 Jul 31 347-352 -
Tunable, ultrasensitive pH-responsive nanoparticles targeting specific endocytic organelles in living cells
Zhou K, Wang Y, Huang X, Luby-Phelps K, Sumer BD, Gao J Angewandte Chemie - International Edition 2011 Jun 50 6109-6114 -
Nanoscopic micelle delivery improves the photophysical properties and efficacy of photodynamic therapy of protoporphyrin IX
Ding H, Sumer BD, Kessinger CW, Dong Y, Huang G, Boothman DA, Gao J Journal of Controlled Release 2011 May 151 271-277 -
Shape-specific polymeric nanomedicine: Emerging opportunities and challenges
Tao L, Hu W, Liu Y, Huang G, Sumer BD, Gao J Experimental Biology and Medicine 2011 Jan 236 20-29 -
Clinical applications of heme biosynthetic pathway: Photodynamic therapy with protoporphyrin IX
Ding H, Sumer BD, Gao J 2011 Jan 197-210 -
Patterns of regional metastasis in advanced stage cutaneous squamous cell carcinoma of the auricle
Peiffer N, Walter K, Myers LL, Isaacson B, Sumer BD, Truelson JM, Ahn C, Roland PS Otolaryngology - Head and Neck Surgery 2011 Jan 144 36-42 -
Head and neck cancer
Crozier E, Sumer BD Medical Clinics of North America 2010 Sep 94 1031-1046 -
In vivo angiogenesis imaging of solid tumors by αvβ 3-targeted, dual-modality micellar nanoprobes
Kessinger CW, Khemtong C, Togao O, Takahashi M, Sumer BD, Gao J Experimental Biology and Medicine 2010 Aug 235 957-965 -
Polymeric micelle nanoparticles for photodynamic treatment of head and neck cancer cells
Cohen EM, Ding H, Kessinger CW, Khemtong C, Gao J, Sumer BD Otolaryngology - Head and Neck Surgery 2010 Jul 143 109-115 -
Microvascular flap reconstruction of major pharyngeal resections with the intent of laryngeal preservation
Sumer BD, Gastman BR, Nussenbaum B, Gao F, Haughey BH Archives of Otolaryngology - Head and Neck Surgery 2009 Aug 135 801-806 -
Correlation between intraoperative hypothermia and perioperative morbidity in patients with head and neck cancer
Sumer BD, Myers LL, Leach J, Truelson JM Archives of Otolaryngology - Head and Neck Surgery 2009 Jul 135 682-686 -
Interdigitating dendritic cell sarcoma of the parotid gland: case report and literature review
Efune G, Sumer BD, Sarode VR, Wang HY, Myers LL American Journal of Otolaryngology - Head and Neck Medicine and Surgery 2009 Jul 30 264-268 -
Changing patterns of tracheotomy use in anterior skull base surgery with free tissue reconstruction
Myers LL, Sumer BD, Lowery JE, Truelson JM, Leach JL, Sinard RJ Laryngoscope 2009 Mar 119 453-458 -
Multifunctional micellar nanomedicine for cancer therapy
Blanco E, Kessinger CW, Sumer BD, Gao J Experimental Biology and Medicine 2009 Feb 234 123-131 -
Free tissue transfer reconstruction of the head and neck at a veterans affairs hospital
Myers LL, Sumer BD, Defatta RJ, Minhajuddin A Head and Neck 2008 Aug 30 1007-1011 -
Theranostic nanomedicine for cancer
Sumer B, Gao J Nanomedicine 2008 Apr 3 137-140 -
Characteristics of sensorineural hearing loss in children with inner ear anomalies
Coticchia JM, Gokhale A, Waltonen J, Sumer B American Journal of Otolaryngology - Head and Neck Medicine and Surgery 2006 Jan 27 33-38 -
Caspase inhibition enhances ischemic tolerance of fasciocutaneous flaps
Sumer BD, Gastman BR, Gao F, Haughey BH, Paniello RC, Nussenbaum B Laryngoscope 2005 Aug 115 1358-1361
-
Supportive Care Needs Among Pretreatment Head and Neck Cancer Patients According to Smoking Status: A Cross-Sectional Study With Nested Analyses
Research
- Nanotechnology
- Cancer metabolism
- Cancer immunotherapy
- Image-guided surgery
- Cancer imaging
Clinical Focus
- Head & Neck Cancers
- Transoral Robotic Surgery
- Surgical Treatment of Head & Neck Cancers
- Transoral Laser Surgery
- Surgical Treatment of Benign Head & Neck Conditions
- Medical Treatment of Head and Neck Cancer
- Skull Base Surgery
Q&A by Dr. Sumer
Articles by Dr. Sumer
Otolaryngology Clinic
at West Campus Building 3 2001 Inwood Road, 6th and 7th FloorDallas, Texas 75390 214-645-8898 Directions to Otolaryngology Clinic at West Campus Building 3, Dallas Parking Info for Otolaryngology Clinic
New Patient Appointment Accepting Virtual Visits or 214-645-8898