Good news on COVID-19 vaccines for pregnant moms, early data shows
May 18, 2021

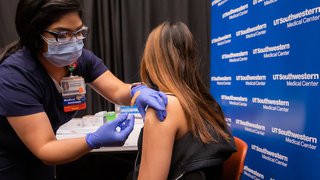
When the COVID-19 vaccine rollout began, there was a lot of uncertainty about what providers should recommend for pregnant patients and lactating patients, who were excluded from the vaccine clinical trials. So, we had to use our knowledge of the science behind the vaccine development and our past experiences with similar vaccines to make recommendations.
Our professional societies – the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine – stepped up. Both emphatically said women who want to receive the vaccine should be allowed to get it.
Fortunately, we gained a lot of experience in the months that followed, and medical organizations have started to publish their data. Having this information should give patients confidence in making their decision to get vaccinated. Recent publications have covered the topics of safety in pregnancy, passive protection to the fetus and hence the newborn, and the presence of antibodies in breastmilk.
Here are three highlights from this research that we want all pregnant patients to know about.
Are you ready to get vaccinated? Schedule your COVID-19 vaccination appointment now.
1. COVID-19 vaccines safe in pregnancy, preliminary clinical trial data suggest
Vaccine trials that include pregnant women are underway. Researchers are also gathering more information about the safety of mRNA vaccines administered to pregnant women.
There are three primary sources of information:
- V-safe After Vaccination Health Checker is a voluntary surveillance system from the Centers for Disease Control and Prevention (CDC). Thousands of people signed up for this smartphone app after receiving their first dose of one of the COVID-19 vaccines. V-safe follows patients for 12 months after vaccination and sends them messages to gather data about side effects, symptoms, and infections. The system also asks whether the enrollee is pregnant, and it can track that data separately.
- V-safe Pregnancy Registry is a database that collects more detailed information about pregnancy and neonatal outcomes. Some women were contacted by the CDC to consider being part of this database.
- Vaccine Adverse Event Reporting System (VAERS) is a national early reporting system designed to capture signals that might indicate a problem with a certain vaccine. For example, this reporting system was used to review cases of cerebral sinus thrombosis associated with the Johnson & Johnson/Janssen COVID-19 vaccine.
What these systems have taught us so far
V-safe data showed that pregnant women experience similar symptoms to non-pregnant women following receipt of the mRNA vaccines: local pain at the injection site, fatigue, headache, and muscle aches.
Less than 1 percent of women reported a fever after the first dose, and 8 percent reported a fever with the second dose, according to preliminary data published in the New England Journal of Medicine. If you develop a fever after receiving the vaccine, you can take acetaminophen (Tylenol), but there is no need to take it before getting the shot.
Health care workers (HCWs) made up 94% of participants in the first three months of the V-safe Pregnancy Registry. This makes sense because early access to the vaccine was limited to HCWs and people at high risk for adverse outcomes.
Women reported receiving vaccinations from around the time of conception through the third trimester. Although we can’t make precise comparisons, frequencies of fetal loss, preterm birth, and anomalies in the V-safe Pregnancy Registry appear similar to data in other published reports.
There have been a few adverse event reports filed with VAERS regarding pregnant patients. About two-thirds of these are non-pregnancy-related events (such as fevers). No birth defects were reported. The most common pregnancy-related complication reported is miscarriage, which was reported by 46 of 221 patients (20 percent) who reported complications.
While this information is not conclusive, it certainly can be viewed as reassuring. Across these systems, there are no signals suggesting that vaccination during pregnancy is not safe.
2. Antibodies transferred from vaccinated moms to fetuses across placentas
An April 2021 study in Obstetrics & Gynecology reported outcomes for 122 women who had received one or two doses of the Pfizer or Moderna vaccine while pregnant. The women had not previously had a COVID-19 infection and tested negative for infection at delivery via a PCR test.
The researchers looked for the presence of antibodies in the umbilical cord blood after delivery to determine whether protective antibodies had transferred across the placenta to their infants:
- 44 percent of infants had detectable antibodies in the blood after a single dose of vaccine.
- 99 percent of newborns had antibodies after their mothers had two doses of vaccine.
- The level of antibodies in the mother’s blood increased over time, and so did the transfer of antibodies to the fetus.
- The earliest the antibodies showed up in the cord blood was 16 days after the first dose, which suggests that women wanting to provide protection to their newborn should be vaccinated at least a few weeks before delivery.

3. Babies can get antibodies from vaccinated woman’s breast milk
Researchers in a March 2021 study in the American Journal of Obstetrics and Gynecology looked for the presence of antibodies in the blood and breastmilk of 131 lactating women who received the vaccine.
Samples were collected at the time of the first vaccine dose and the second dose and then two to six weeks after the second dose, when there should be maximal antibody production.
The researchers determined that these women developed robust responses in their blood to the vaccine and that antibodies in their breast milk also increased with vaccination. Importantly, there was a significant increase in the level of antibodies contained in breast milk following the second dose of the vaccine.
As more people in the U.S. get vaccinated against COVID-19, we anticipate reporting of more useful data regarding long-term outcomes for pregnant patients who chose to be vaccinated.
Though not conclusive, preliminary data align with the recommendations of ACOG, SMFM, and the CDC: The vaccine appears to be safe in pregnancy and lactation, and patients who want to be vaccinated against COVID-19 while pregnant or lactating should be allowed to do so.
These and future clinical studies contribute to our knowledge about vaccine safety and efficacy in pregnant and lactating women. If you have questions or concerns, please talk with your Ob/Gyn or health care provider. We are here to help you make informed decisions about your pregnancy-related health care.
To visit with an Ob/Gyn, call 214-645-8300 or request an appointment online.