Reaching the summit after hip dysplasia surgery: Cynthia's story
June 26, 2020

Cynthia Porcari is a cardiothoracic operating room nurse at William P. Clements Jr. University Hospital. Five years ago, a twinge of hip pain sent her on an uphill battle with hip dysplasia, a condition most people think only affects dogs.
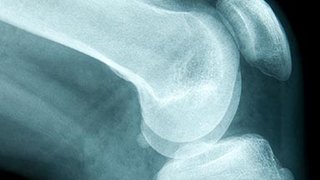
Essentially, her hip socket was not deep enough to support the ball of her hip, which led to constant, progressive pain. Adult hip dysplasia is the leading cause of hip arthritis before age 50.
Approximately 90% of patients with hip dysplasia are diagnosed as teens or young adults. But in the other 10%, the symptoms can be so mild that early diagnosis can slip by. That's what happened to Cynthia.
Her pain crept up for several years, then, within weeks, simple movements became unbearable. Cynthia was forced to give up her annual hiking trip to Colorado. At the peak of her struggle – and around the time I joined the UT Southwestern Orthopaedic Surgery team – she, at age 40, relied on a cane to walk longer distances.
Two years later, Cynthia's life is dramatically different. After undergoing a complex surgical procedure known as periacetabular osteotomy (PAO), in which the hip bones are cut and the socket is repositioned, the biomechanics of Cynthia’s hip are sound. And following a regimen of diligent, daily physical therapy, she has reclaimed her mobility.
Now, Cynthia leans on her experience to help others who are suffering with adult hip dysplasia. Cynthia's a great storyteller – she, along with my clinical assistant Adina Stewart, help with social media and content creation for Miles4Hips, a hip dysplasia awareness organization.
June is Hip Dysplasia Awareness Month, so I've invited Cynthia to share her story, as only she can tell it.
My hip dysplasia story: 5 years, 3 surgeries, and a trip to Boston
By Cynthia Porcari, BSN, RN, CNOR

I got out of bed one morning in early 2015, and I noticed pain in one of my hips. I probably pulled a muscle at the gym or at work, I thought. As a nurse, I'm constantly moving up, down, and all around during shifts.
And I knew it couldn't be aging pains. I was just 38 at the time.
The hip pain continued, morning after morning, and it started to hurt when I made simple movements like getting in the car. I knew something wasn’t right, and I was heartbroken. There was no way I'd be able to take my annual hiking trip to the Colorado Rockies – I could barely even sit without pain.
A 10-hour car ride that fall was the last straw. In lieu of the mountains, I took a trip to the beach. My thought was that walking on soft sand would be gentler than climbing a rocky trail.
But the drive had been agonizing, and my walk devolved into a persistent limp.
From nurse to patient
After vacation, a co-worker saw me limping and suggested I see a sports medicine doctor. I took the advice, and was diagnosed with two conditions that often go hand-in-hand:
- Femoroacetabular impingement (FAI), when the ball-shaped part of the femur doesn't sit right within the hip socket.
- And a tear in the labrum, the cartilage that lines the hip socket.
In spring 2016, I had arthroscopic hip surgery, also known as a scope, to repair the torn labrum. The surgeon made small incisions to see inside the hip joint with an imaging device and insert tiny tools he'd use to shave the bone and fix the tear. I felt better for a little while after the scope, but in late 2016, my hip pain returned with a vengeance.
I tried physical therapy to rebuild my strength, but the pain kept getting worse over the next year. We even tried a steroid injection, but nothing helped. My limp returned at work – not great for a nurse who walks about 10 miles a day.
A second scope was recommended, and I was referred to Joel Wells, M.D., M.P.H., for a second opinion. Dr. Wells has extensive experience with hip pain disorders and procedures. He had joined UT Southwestern just a few months earlier – talk about perfect timing!
A ‘tricky’ diagnosis: Hip dysplasia
At my first visit, Dr. Wells suggested that I might have hip dysplasia. He said my case was "tricky" for several reasons:
- My condition was mild, and I had a bone spur.
- I was 41 – much older than most patients who are diagnosed with hip dysplasia.
- Non-invasive imaging alone could not confirm the cause of my pain.
He agreed on trying the second scope. So, I had that procedure with my previous surgeon in early 2017. The surgeon hoped that cleaning up the inflamed area, repairing the probable tear, and following a specialized physical therapy plan would help me recover. But it didn't do the trick. Though I exercised diligently, I had to start using a cane when I wasn't at work.
Aside from total hip replacement, the only option to correct my hip dysplasia was an advanced procedure called periacetabular osteotomy. While PAO can dramatically improve hip dysplasia pain, it's a major surgery that involved cutting the bones and repositioning them with screws. Dr. Wells suggested I get a second opinion from one of his mentors, Michael Millis, M.D.
I never dreamed I would fly across the country for a second opinion, but I couldn't tolerate the pain and lost mobility anymore. So, in late 2017, I got on a plane and braved the winter weather in Boston.
Ultimately, the trip was worth it. Dr. Millis agreed that PAO was the best option. After hearing from both doctors, I decided to move forward with the procedure. And it was just in time:
My ankles and knees were aching due to my unnatural gait. My pain had reached maximum threshold. I needed relief, and the surgery seemed like the only way to get my life back.
'In summer 2019, I made my triumphant return to hiking with a 10-mile route through the Colorado Rockies. I wasn't the fastest person on the trail, but I felt great – physically and emotionally. The view was breathtaking; I never would have experienced it again without Dr. Wells and PAO.'
Cynthia Porcari, BSN, RN, CNOR
PAO: A major hip dysplasia surgery
For a month or so prior to surgery, Dr. Wells helped me optimize my health with a high-protein diet and strength training. A patient can lose 1% to 1.5% of muscle strength daily when they're sedentary due to surgery or illness. Every patient recovers from PAO differently, and we wanted to avoid potential obstacles.
Dr. Wells described PAO to me as a "Goldilocks" surgery – you want just enough movement in the hips, but not too much.
I had the PAO surgery in April 2018. Dr. Wells used advanced imaging to plan the route of the surgery. It's not yet a robot-assisted surgery, but Dr. Wells said that's one of the advances he hopes to see in the next few years.
Then he did the procedure via intraoperative fluoroscopy, a special X-ray technology that allowed him to guide surgical instruments through a small incision in my hip to operate inside and between the bones of my hip joint.
The hip joint is made of the femoral bone (the ball) and the acetabulum (the socket, which is part of the pelvis). Dr. Wells made four incisions in the bone around my socket to free up the hip joint while keeping my pelvis stable. In doing so, he totally changed the mechanics of my hip without detaching any muscle or disturbing any of the delicate nerves.
When I woke up, my leg felt extremely heavy, and I was in a lot of pain. Thankfully, the amazing nurses helped me get that under control quickly.
I hadn't walked without limping in three years, and I was so stiff those first few days after the PAO, so I couldn't help worrying about whether the procedure had really worked: What if I never regain my full mobility? What if I couldn't continue working as an OR nurse? What if I had to give up hiking for good?
But Dr. Wells and his team reassured me I would get there in my own time. Three days post-surgery, I was able to walk down the hall with assistance. I stayed three nights in the hospital, then my mom took me to her house to continue recovering. I also did daily physical therapy exercises at UT Southwestern Sports Medicine, which I continue to do at home. Physical therapy is a lifelong commitment after PAO surgery.
The first two weeks of recovery were the most difficult, and I needed a lot of help. Then, between the second and third weeks, I became more independent.
By six weeks after surgery, I was cleared to bear weight. At nine weeks, I could walk some with a cane. By 10 weeks, I could walk short distances without a cane. Finally, at 12 weeks, I only needed the cane for long-distance walking.

Over the next year, I got stronger day by day. In summer 2019, I made my triumphant return to hiking with a 10-mile route through the Colorado Rockies. I wasn't the fastest person on the trail, but I felt great – physically and emotionally. The view was breathtaking; I never would have experienced it again without Dr. Wells and PAO.
Throughout the preparation and recovery, Dr. Wells and his team checked in with me frequently. They are very focused on their patients’ clinical outcomes. He wanted to know how I really felt about the procedure and my recovery.
In fact, he's creating a hip database filled with patient data and experiences to help guide other doctors around the world learn from the people who have lived those outcomes.
Helping others through Miles4Hips
Before surgery, I basically I went to work, then home, then work again, and that was it. Now, I can go to the gym, take walks, and take care of my patients with hardly any pain.
While I'm thrilled to be active again, the best part of this journey has been the chance to help others with hip dysplasia. Dr. Wells, his fantastic clinical assistant Adina, and I all volunteer with Miles4Hips, a collaboration between patients and the International Hip Dysplasia Institute. Miles4Hips means that hip dysplasia is a journey, from diagnosis through treatment, recovery, and beyond.
We attend meetings, help with awareness events, and translate clinical data and patient experiences into impactful stories. Our goal is to help people avoid unnecessary pain and get the right care to increase their quality of life.
Life's too short to live with debilitating hip dysplasia. I encourage anyone with chronic hip pain to ask for a referral to a specialist like Dr. Wells. Getting better was an uphill climb, but it’s a beautiful view from the top!
To schedule a hip pain consultation, 214-645-8300 or request an appointment online.