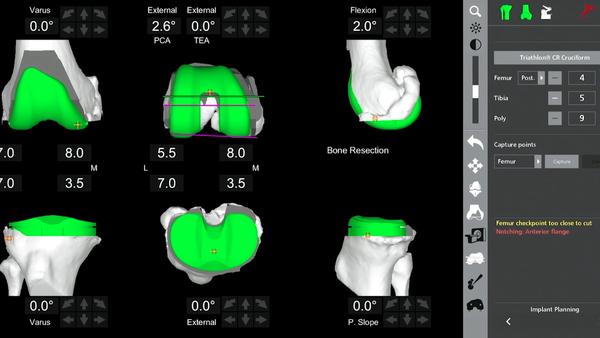
Two-stage knee fusion surgery restores mobility for Texas woman with obesity
April 23, 2026
Obesity impacts much more than a patient’s metabolic and emotional health. It also creates layers of medical complexity that affect daily life, particularly mobility. When it hurts to move, people are less likely to exercise, which leads to additional weight gain. It’s a vicious cycle that can crush a person’s independence and fast-track joint degeneration.
People with obesity are 20 times more likely to undergo a knee replacement, but standard prosthetics are not designed to support heavier weights. Plus, obesity-related conditions such as high blood pressure, Type 2 diabetes, and obstructive sleep apnea can increase the risk of surgical complications.
Many patients wind up seeing multiple doctors for repeated surgeries that ultimately fail. When the prosthetic breaks or the tissues become infected, patients are often left with two dismal options: live with immeasurable pain or have the leg amputated.
But there may be another option.
Orthopedic surgeons can help people avoid amputation by looking beyond their current health status – seeing the patient as a person, not as a diagnosis or a liability. We did just that for a woman who came to the UT Southwestern Medical Center as a last attempt to save her leg from amputation.
This Texas grandmother had severe obesity, with a body mass index (BMI) of 75 – more than double that of the average U.S. adult. After a failed knee replacement at another hospital in 2018, she suffered through six more unsuccessful surgeries that left her with progressively worsened pain and mobility. Bed-bound, she needed help to bathe and use the bathroom. She was depressed and vulnerable to pressure sores, urinary tract infections, rapid muscle deterioration, and loss of bone density (osteoporosis).
Though she was told elsewhere that amputation was her only option, neither she nor the UT Southwestern Orthopaedic Surgery team were willing to accept that fate. We designed a two-stage knee fusion procedure and a custom knee prosthetic that could support her weight through recovery and in the long-term.
Today, this patient always gives me a big hug when she walks confidently into her follow-up appointments. Though her leg can no longer bend, she is mobile and no longer living in bed. Her pain is under control, she’s losing weight, and, best of all, she can play with her grandchildren again.
For her, the knee-fusion surgery was more than limb-sparing. It was lifesaving.
Stage 1: Out with the old hardware
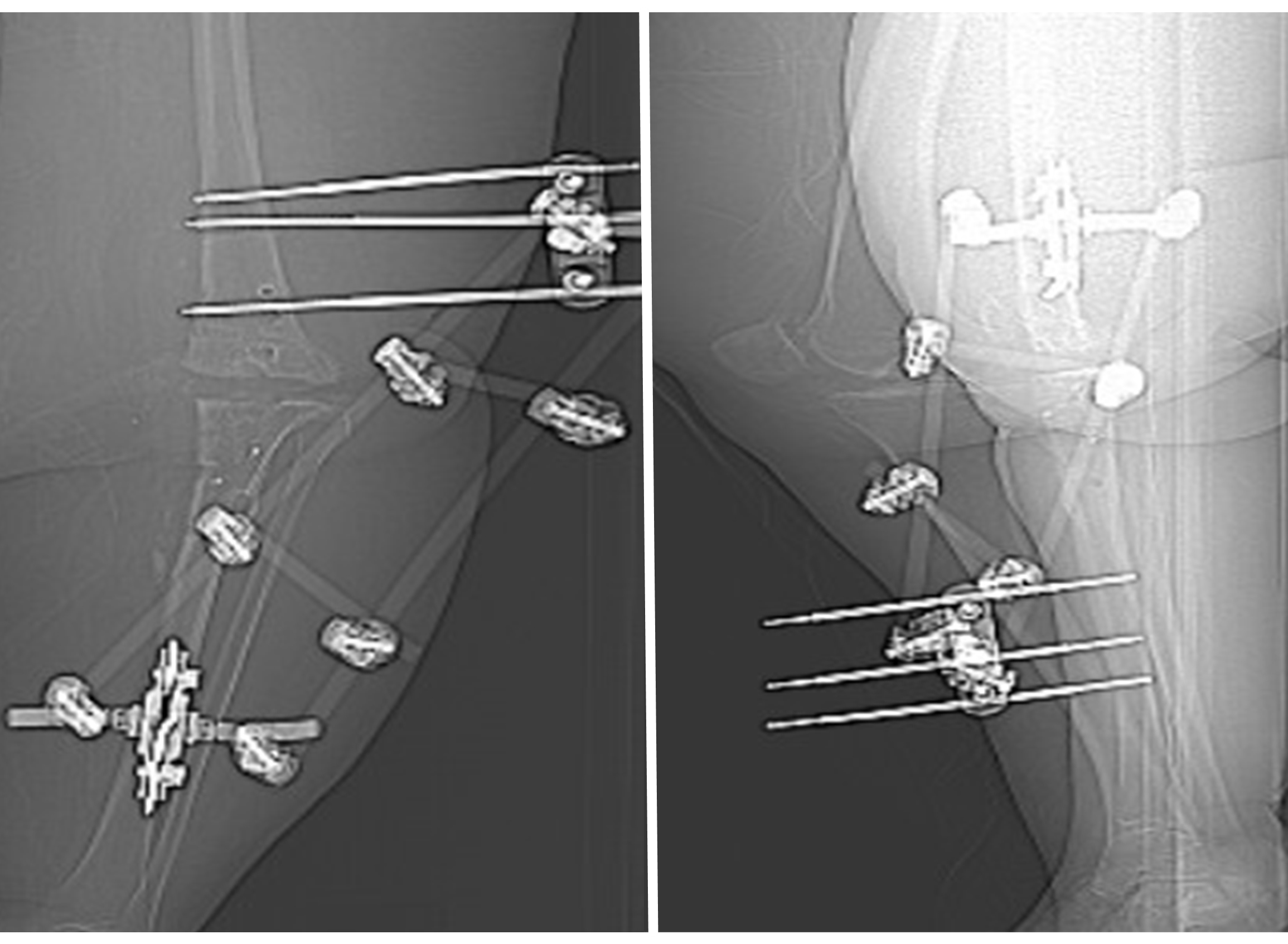
We confirmed through imaging that the patient had enough bone and soft tissue remaining in her knee area to attach the prosthesis. We also discovered that she had relatively small bone structure for her size, emphasizing the need for a custom device.
Standard joint replacement implants are not designed to withstand the weight of a person with severe obesity, let alone the force of walking or exercising on them. The American Academy of Orthopaedic Surgeons recommends a BMI limit of 40 for patients seeking total knee arthroplasty (knee replacement) – about half of our patient’s BMI. The cutoff is recommended due to increased risk of poor outcomes data and complications such as blood clots, rehospitalization, and infection.
Our orthopedic surgeons thought that if we could plan strategically, starting with a clean slate, we could offer this patient a chance for better outcomes.
To begin, we removed the failed prosthetic, plates, and screws from past surgeries. While this is a normal part of revision joint surgery, this patient’s surgery was more complicated and took two to three times longer due to the volume of tissue we had to work through to access the joint and hardware.
During the procedure, we placed slow-releasing antibiotic beads near an infection discovered in the patient’s knee. We also installed an external fixator device to provide more stability for her leg during the waiting period while her custom knee implant was designed.
Custom-made implant for a unique patient
If you’re buying a new car off the lot, you can usually get one right away. But our patient wasn’t getting a standard Mustang. She needed a custom-built Ferrari, which takes time and planning.
With CT scans of our patient’s knee in hand, we met with a team of engineers at a leading custom prosthesis company that we regularly partner with. The engineers used CAD/CAM software with the patient’s imaging and overlaid it with computer-generated graphics to design the device. Our goal was to create an implant narrow enough to fit within the patient’s smaller bones but strong enough to support her weight as the femur (thigh bone) and tibia (shin bone) fused into a stable structure.
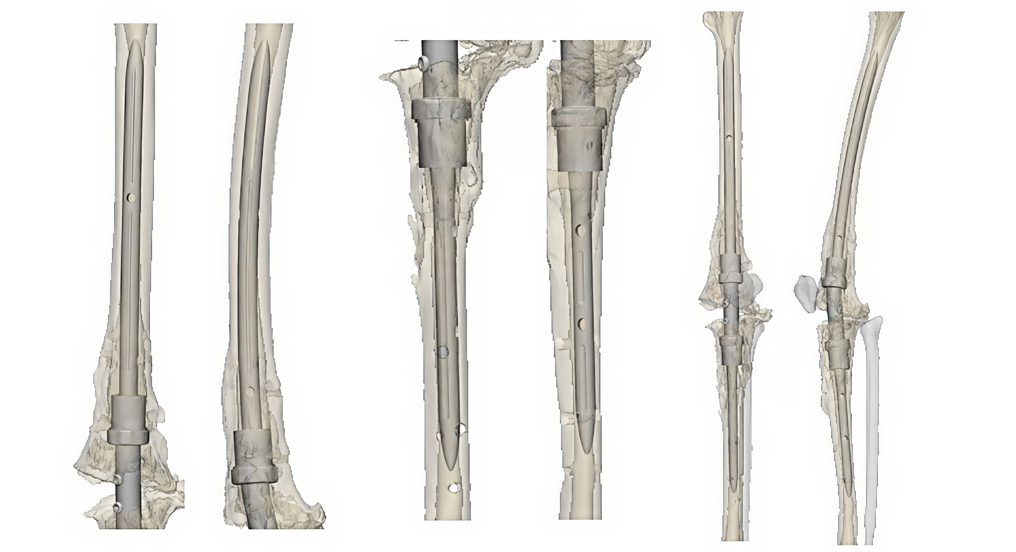
In a typical knee fusion (arthrodesis), we place a metal rod inside the bones from the top of the hip to the ankle, creating stability. The rod is usually one piece, and the smallest rods are around 12 millimeters wide (0.4 inches). We would then access the patient’s leg from the hip and guide the rod down the leg bones to the ankle.
But because of this patient’s size, we would have had to go through several inches of tissue to access her hip bone, extending the surgery and increasing the risk of complications. The leg bones are wider at the ends and narrow in the middle – even the smallest off-the-shelf rod would not have been able to fit inside her bones and support her weight. The knee area, where the femur and tibia would eventually connect, is both the narrowest place and the spot that absorbs the most weight-bearing stress.
She needed a wider rod to hold her weight, but it had to be narrow enough to fit inside her small bones. In our brainstorming session, we envisioned a two-piece rod that could be inserted lower in the leg and fortified in the middle upon insertion.
The engineers tapered the ends of each piece and designed them to overlap at the knee area, creating a larger, sturdier surface area called a lap joint. The overlap bulked the rod in the middle – its strength quadrupled with each extra millimeter of width. The engineers also designed a 3D-printed implant to aid fusion of the femur and tibia.
Our orthopedic surgeons at UT Southwestern perform more than 450 knee replacement surgeries each year, and we are among the top U.S. hospitals for orthopedic care. Because of our volume and the complexity of cases, we’ve formed professional relationships with leading device companies that can fast-track custom prosthesis design.
For our patient, this waiting period was the hardest part. We talked frequently as she transitioned between nursing homes and her own home due to insurance challenges. Throughout that trying time, she remained focused on her goals: salvage the leg and regain mobility.
Stage 2: In with the new custom implant
The patient was placed under general anesthesia for the knee fusion surgery. Our expert anesthesiology colleagues monitored her throughout the lengthy procedure – patients with obesity are at increased risk of complications with breathing, venous access, and blood pressure during sedation.
Rather than accessing her leg bones through the hip, we guided one custom rod through her knee and upward into the femur and the other rod from the knee to the ankle. The rods overlapped in the middle at the bolstered lap joint, and the 3D-printed implant was placed between the original bones.
After surgery, she stayed in the hospital for several days to recover. Having been bed-bound for so long had led to muscle atrophy, and she needed significant physical and occupational therapy with our Physical Medicine and Rehabilitation team. She put in months of exercises to build strength and learn how to walk on a non-bending leg.
Less pain, more joy
The two-stage knee fusion surgery saved this patient’s life. She no longer faces a grim future of bed-bound comorbidities and round-the-clock care. With her newfound independence, she is losing weight and chipping away at her obesity-related health risk factors.
By bringing compassion, expertise, and the most advanced, custom-designed technology to the table, we were able to help significantly improve this patient’s pain and mobility. It was humbling to be a part of her journey to claim a new lease on life.
To talk with an expert about complex knee replacement or revision, make an appointment by calling 214-645-3300 or request an appointment online.