Expertise in Ex Vivo Lung Perfusion
For some patients with certain serious lung diseases, lung transplantation is the only treatment that can save their lives. However, patients often must wait for weeks or months for transplant because only about 20 to 30 percent of donor lungs are usable.
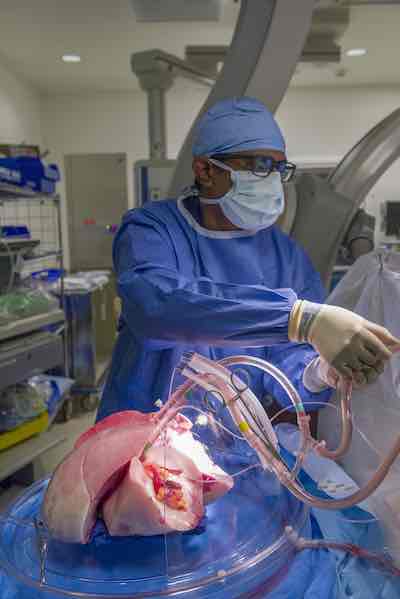
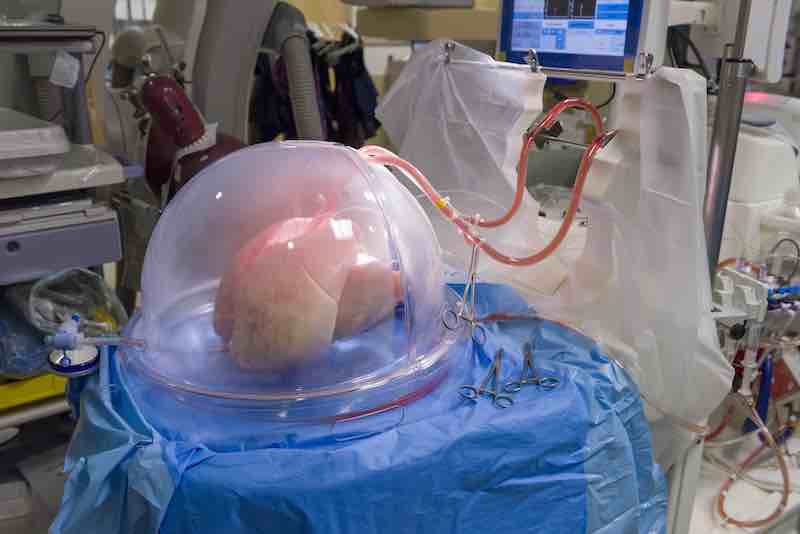
Ex vivo lung perfusion (EVLP) is technology that helps to assess and possibly repair and restore lungs that are damaged at the time of the donor’s death. By repairing lungs that might have previously been considered too damaged for transplant, EVLP helps expand the pool of healthy donor lungs – and helps us save additional lives.
UT Southwestern’s lung transplant team performs more than 60 lung transplantations each year and is one of fewer than two dozen U.S. centers using EVLP. Our team consists of pulmonologists, surgeons, cardiologists, transplant coordinators, nurses, dietitians, social workers, and pharmacists – providing a multidisciplinary approach to caring for patients with end-stage lung disease who need transplantation. Our multidisciplinary approach helps us deliver a personalized treatment plan for each patient that includes postoperative and long-term care.
Conditions We Treat
Lung transplantation is a treatment for people with end-stage lung disease for whom other treatments have failed. Our lung transplant specialists typically recommend transplantation for people with severe lung diseases such as:
Treatment With Ex Vivo Lung Perfusion
At UT Southwestern, we use the EVLP system as part of our lung transplantation process. The system helps our transplant team more thoroughly evaluate donor lungs and improves the quality of donor lungs as they are being considered for transplantation.