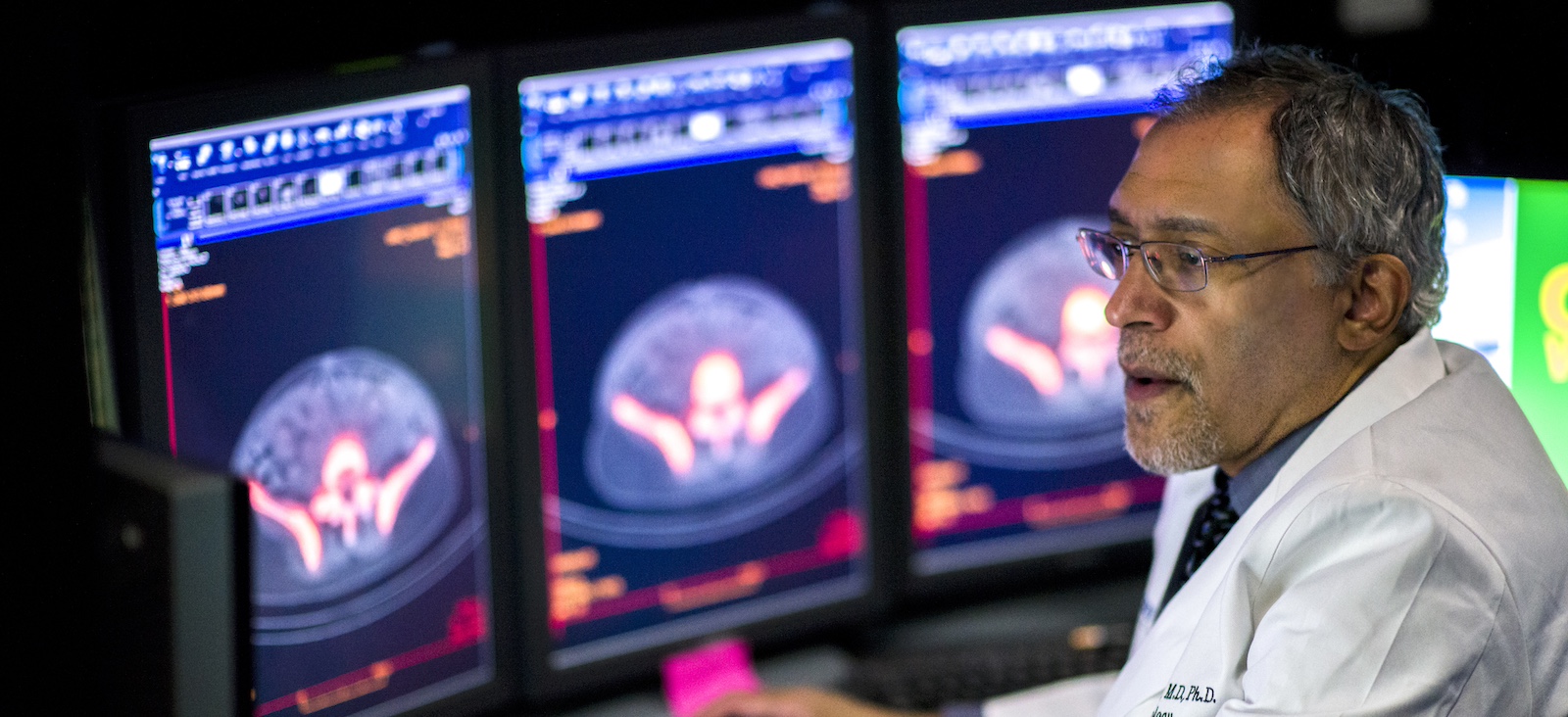
State-of-the-art treatment combines therapy, diagnostics
UT Southwestern offers a specialized molecular targeted therapy known as theranostics for patients like Maria Hernandez. “First, we will make the diagnosis so we will be able to detect where the cancer is and then we give the therapeutic isotope to treat the cancer,” said Martin Pomper, M.D., Ph.D., Chair and Professor of Radiology at UT Southwestern. “It’s been shown to be much less toxic than a lot of other ways of treating cancer.”