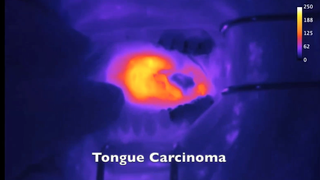
The middle ear is filled with tiny, delicate structures that affect hearing, balance, and facial movement. While most middle-ear problems aren’t life-threatening, they can greatly affect your quality of life.
A hole in the ear drum or a skin cyst can result in infections, causing damage to the ear bones and nearby structures. Without proper treatment, middle-ear conditions can cause serious complications such as hearing loss, facial paralysis, balance problems, or brain infections such as meningitis, which can be life-threatening.
Surgery for middle-ear disorders can help reduce symptoms and preserve hearing. Depending on your condition, your doctor may recommend either traditional open surgery using a microscope or a minimally invasive approach called transcanal endoscopic ear surgery (TEES).
Traditional surgery involves a small incision, usually 2 inches or less, behind the ear to access the problem area. TEES requires no external incisions. It uses a high-definition, lighted endoscope – a thin, narrow tube with a light at the tip – to address the issue through the ear canal.
These types of ear surgery have been proven safe and effective for common and rare middle-ear conditions, and UT Southwestern is a leader in both. We perform hundreds of ear surgeries every year for adults and children with complex ear disorders.
As a high-volume surgery center, we have the expertise to recommend the type of surgery that will give you the best outcome for your specific condition. While endoscopic surgery can offer some benefits for patients, it may not always be the best approach.
We’ve highlighted the differences between traditional and endoscopic ear surgery, along with information to help you make informed decisions about your care.
What is traditional ear surgery?
With traditional ear surgery, the surgeon makes an incision behind the ear to lift it away from the mastoid bone – a projection behind the bottom tip of the earlobe. In some cases, we also must open the bone. From there, we can access the middle ear from the back.
Using a high-powered microscope, we can get a real-time, 3D visualization of the structures of the ear. Traditional ear surgery techniques have been used since the 1920s. There are decades of research to show that this approach is safe and effective for many types of middle-ear conditions.
Advantages: Using this approach, the microscope is mounted above the patient’s head so the surgeon can use both hands to maneuver the surgical tools and remove blood and fluids from the area during the procedure.
The surgeon will hide incisions in the hairline or among the natural curvatures of the head when possible. In general, the external incisions are small and not very noticeable.
Disadvantages: Microscopes provide a straight-line view; we cannot see around corners or into hidden spaces of the middle ear space without creating incisions outside the ear. In some cases, surgeons must create bigger incisions to access the source of the problem.
What is TEES?
Using a high-definition endoscope, we can access internal ear structures by placing the scope through the ear canal rather than making an external incision. Its camera provides a close-up view of the damaged area and a wider visualization of areas that an external microscope can’t see.
Advantages: The flexible endoscope can show us around the corners, nooks, and crannies of the middle ear from the inside, making access to disease better. Patients also may heal faster and with less pain during recovery from TEES.
Ongoing research, including by UTSW otolaryngologist Daniel Killeen, M.D., is comparing the difference in post-surgery discomfort between the two approaches. The findings will help guide us in creating evidence-based surgical plans going forward.
“Because of the improved visualization, the endoscope enables me to perform more surgery through the ear canal as opposed to making an incision behind the ear,” Dr. Killeen notes. “Ultimately, excellent outcomes can also be obtained with the microscope and without the endoscope – I recommend trusting the discretion of the surgeon for which approach is best for your ear.”
Rance Fujiwara, M.D., implements TEES when possible, noting, “It gives me a superior view and access to disease that is often better than with a microscope.”
Disadvantages: Unlike the two-handed method with traditional ear surgery, a surgeon performing TEES must hold the endoscope with one hand. That means they have only one free hand to maneuver the surgical equipment.
Though the endoscope can show more of the hidden areas of the ear, it provides a two-dimensional visualization instead of 3D, similar to watching a video game on a screen.
While these are not necessarily negatives, TEES is a specialized approach that requires an experienced surgeon. UTSW has offered TEES for over a decade. Brandon Isaacson, M.D., who has performed hundreds of endoscopic ear surgeries, says we are “one of the leading centers in the country” in TEES expertise. He serves on the executive board of the International Working Group on Endoscopic Ear Surgery (IWGEES), which promotes the technique and teaches it to interested surgeons around the world.
What conditions can be treated with TEES?
Depending on the location and severity of your ear condition, your surgeon will recommend either traditional ear surgery or TEES – both approaches are proven safe and effective. Some of the conditions we frequently treat with TEES include:
- Canaloplasty, a procedure to widen a narrowed ear canal.
- Tympanoplasty, a surgery to repair a torn eardrum. We see patients three weeks after surgery for a checkup, and most who’ve had endoscopic surgery are already healed.
- Replacement of the ossicles or stapes bones in the ear with miniature prostheses.
- Reconstruction of congenital anomalies in the middle ear that cause hearing loss.
- Stopping cerebrospinal fluid that has leaked into the ear.
- Removal of problematic tissues:
- Benign or cancerous tumors, including facial nerve tumors, glomus tumors, acoustic neuromas (vestibular schwannomas), and paragangliomas.
- Cholesteatoma, a collection of skin and dead skin cells in the middle ear that can become infected.
There are several other common, rare, and complex conditions we can treat with TEES. Browse a list of conditions we can treat endoscopically.
The future of ear surgery
The magnification power and resolution of today’s thinner, more flexible endoscopes is light years ahead of the devices available a decade ago. Modern microscopes also provide crisper, more enhanced images than older machines could. UTSW uses the most advanced equipment to give our surgeons the advantage of superior visualization.
If you need surgery for a middle-ear condition, talk with your surgeon about the approach they plan to use. There are some cases in which traditional surgery is the best option, and sometimes we must switch from endoscopic to traditional surgery during the procedure.
UTSW ear surgeons will recommend the surgical approach that will give you the best outcomes. We welcome your questions, and we will discuss all your options to help you make an informed treatment decision.
To talk with an expert about endoscopic ear surgery, make an appointment by calling 214-645-8898 or request an appointment online.