Advanced sinus surgery relieves nasal polyp symptoms – without a long recovery
October 18, 2021

Most of us have experienced the temporary misery of a stuffy nose or sinuses, especially during cold and allergy season. It can be hard to breathe, smell, and your head may feel as if it weighs a ton. But at least it’s temporary.
For people with chronic rhinosinusitis and nasal polyps, this is their life.
Nasal polyps are noncancerous growths that dangle like grapes from the linings of the nasal passages or sinuses. They can develop in anyone, but approximately 25-30 percent of patients with chronic rhinosinusitis – a persistent, long-term sinus inflammation disorder – develop nasal polyps.
Despite their name, these annoying growths don’t always originate in the nose. Polyps can form in any part of the sinuses, often appearing where the sinuses drain into the nose near the eyes, base of the brain, and cheekbones.
Small nasal polyps may not cause any symptoms, but if they grow large enough, they can block your nasal passages and lead to a host of symptoms, including:
- Runny or stuffy nose
- Difficulty breathing
- Postnasal drip
- Snoring or sleep apnea
- Reduced sense of smell
- Pressure in your face or forehead
Approximately 4% of adults have nasal polyps, which affect twice as many men as women. The growths can make you more susceptible to sinus infections, asthma flare-ups, and sleep apnea.
Historically, sinus surgery has been an ordeal for patients. Outdated techniques such as minimal polyp removal and sinus stripping with nasal packing after surgery produced only short-term results, if any, and often required weeks of painful recovery. Additionally, the commonly advertised “balloon sinuplasty” does not adequately address the underlying inflammation.
But today, there are effective, minimally invasive treatments that can offer immediate and sometimes permanent relief. My colleagues and I at UT Southwestern perform more than 700 advanced sinus surgeries each year, including specialized procedures to remove polyps and widen the delicate sinus passages to reduce and potentially prevent future sinus problems. We also perform revisionary surgery for patients who have had unsuccessful or incomplete surgery in the past.
From personalized medications to state-of-the-art procedures, we have all the tools and are dedicated to finding the best treatment for each patient.
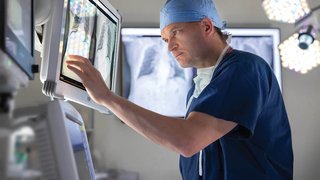
A close-up look at the results of functional endoscopic sinus surgery (FESS)
What causes nasal polyps?
Nasal polyps are the result of chronic inflammation, though we don’t yet understand what triggers them in some people and not others. Certain conditions are shown to increase your risk of developing nasal polyps, including:

- Asthma
- Allergies
- Cystic fibrosis
- Aspirin sensitivity
- Frequent sinus infections
There is not yet a cure for nasal polyps. While we can remove polyps, there is a chance they will return. However, treatment options are becoming more advanced every day, resulting in more days, months, or even years without intrusive nasal polyp symptoms.
What treatments are available for nasal polyps?
When it comes to choosing the best treatment, shared decision-making is key – we will give you all the options and make recommendations for what we think will be most effective for you. However, it is your choice which treatment method to pursue.

Steroid medication
Anti-inflammatory steroid spray is the first line of treatment. Steroids reduce the volume of white blood cells involved in the inflammation that causes nasal polyps.
Medications such as Flonase, Nasacort, or Nasonex, which are also used treat seasonal allergy symptoms, can be delivered straight to the problem area and, because they are given in such small doses, they can be used long term.
One drawback is that nasal steroid sprays can only treat the areas they touch. So, if polyps are hidden within the nooks and crannies within your sinuses, the spray may not reach them.
If nasal sprays do not reduce the inflammation enough, we may recommend an oral or injectable steroid, such as prednisone. This can be highly effective, dissolving polyps and temporarily restoring your sinuses to normal. We rarely recommend long-term use of higher doses of steroids, which can cause serious systemic side-effects such as:
- Osteoporosis
- Cataract formation
- Necrosis of the hip joint
In the past few years, the U.S. Food and Drug Administration has approved a couple of monoclonal antibody medications to treat nasal polyps: dupilumab and omalizumab. These medications, which also treat asthma and some skin conditions, target and knock out one of the molecular pathways of inflammation. However, these medications are expensive, so we recommend them only when other treatments do not work.
Nasal polyps often grow back after they’ve disappeared due to medication or been removed in some surgeries. Because of this, it’s important we find the perfect mix of medical and surgical treatment to get the best results for you over the long term. Doing this requires extensive expertise with the condition. If medication alone does not alleviate your symptoms or the polyps continue to regrow, we may begin to discuss surgery.
Advanced sinus surgery
Sinus surgery has gotten a bad reputation over the years. You may have even heard a nightmare story about it – or maybe you have your own. But today’s sinus surgery, which is called functional endoscopic sinus surgery (FESS), is very different from even 10 years ago.
We no longer strip the sinus lining or insert packing material into the nasal cavity after surgery. If we do need to leave something in the nose, we use material that can be easily vacuumed out or rinsed out with a saline irrigation. We also have much better surgical instruments that are designed for very specific jobs, making the surgery more efficient, effective, and less invasive.
My colleagues and I focus solely on treating sinus diseases, which means we have exemplary knowledge of navigating the delicate sinus cavities and nearby structures: the skull base, brain, carotid arteries, and eye sockets. Because we perform about 700 sinus surgeries a year, 500 of which are just for inflammatory sinus disease, we are experts.
The challenge is to remove polyps and open the sinuses without damaging nearby structures. Surgeons with limited expertise tend not to open sinus cavities wide enough to allow access for future topical steroid treatment. We frequently treat patients who’ve had previous, less effective procedures elsewhere.
At UT Southwestern, which has state-of-the-art operating room equipment, we collaborate with colleagues in other fields, such as neuroradiology, neurosurgery, and ophthalmology.
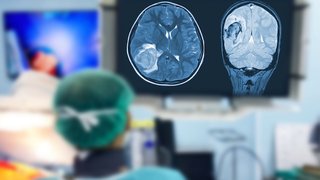
During surgery, real-time 3D CT imaging is displayed throughout the operating room.
We pair sophisticated computer guidance with our surgical expertise to navigate more precisely within the sinuses and remove polyps. The technology adds an additional layer of safety to the surgery, making patients and surgeons more confident in getting positive results.
How sinus surgery works
You will be asleep under general anesthesia during the procedure. In our advanced FESS procedure, we insert an endoscope – a thin, flexible tube with a camera and small tools on the end – into one of your nostrils. The tools allow us to remove nasal polyps under CT guidance and, if necessary, enlarge the openings to your sinus cavities by removing unnecessary walls that create nooks and crannies in which polyps can hide.
After surgery, you should be able to go home the same day – you will need a ride home. Most patients do not feel much pain, but you may have some discomfort, congestion, and spotty nose bleeds for a few days. We recommend using saline washes after surgery to reduce discomfort.
You will need to avoid activities that raise your blood pressure for a couple weeks, including exercise or strenuous activity. Other than that, you can go back to your normal activities within a few days. We recommend that patients take a week off work to rest. However, some patients go back to work the next day.
Patients say the difference between living with nasal polyps and finding the right treatment is like night and day. They can breathe easier and sleep better, which means they can get back to enjoying their lives – and we are honored to be a part of making that happen.
To make an appointment, call the UT Southwestern ENT Clinic at 214-645-8898 or request an appointment online.
Inside the Operating Room During Sinus Surgery



More in: Discovery, ENT, Men's Health