Headlines should not determine your healthcare choices – that sage advice has never proven more valuable than recently, when media coverage of a European clinical trial on colonoscopy screenings incorrectly questioned their effectiveness.
Interim results from the “landmark” NordICC trial, the first randomized clinical study on colonoscopy, were published Oct. 9, 2022, in the New England Journal of Medicine. The research, which involved nearly 85,000 people in Poland, Norway, Sweden, and the Netherlands, contained several valuable scientific findings – the most important of which is that colonoscopy reduces the risk of developing colorectal cancer by 31% and the risk of dying from it by 50% in adults 60 and older.
Unfortunately, those findings were overshadowed by the more controversial and misinterpreted topline result, which indicated that of the people “invited” to participate in the study, there was only an 18% reduction in cases of colon cancer and almost no impact on the risk of death.
Here’s the problem: More than half of the research participants who were “invited” to get the procedure chose not to have one. The trial’s baseline figures included all patients invited to join the study – not just those who participated.
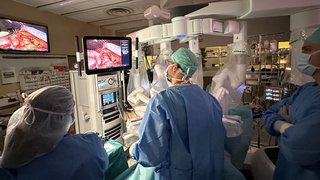
Colonoscopy, a procedure in which an endoscopist inserts a thin, flexible tube with a tiny camera into the rectum and examines the inside of the colon for swelling, irritated tissues, polyps, or cancer, remains the gold standard to detect and remove precancerous polyps. But it only works if a patient actually gets a completed procedure.
"In fact, the trial data confirms that getting a colonoscopy is the best way to reduce the risk of getting colorectal cancer and to detect it early when it is most treatable. But you wouldn’t know that from the headlines."
Roopa Vemulapalli, M.D.
Among the approximately 12,000 participants who did get a colonoscopy, their risk of developing colorectal cancer fell by 31% and their risk of dying from it decreased by 50%. Those numbers are also significant when we compare the vast differences in screening protocols and quality, culture, and diversity between the U.S. and Europe:
- The U.S. has actively reduced the recommended age to start regular screening at 45 for patients at average risk of colon cancer, which has helped steadily decrease colon cancer incidents and death for three decades in adults 50 and older.
- Many European countries begin colon cancer screening later in life. Norway, for example, offers just one lifetime screening colonoscopy between ages 55 and 69 – and they have one of the highest rates of colon cancer in the world.
In fact, the NordICC trial data confirms that getting a colonoscopy is the best way to reduce the risk of getting colorectal cancer and to detect it early when it is most treatable. But you wouldn’t necessarily know that from the headlines. And the timing couldn’t have been worse for questioning data around colon cancer screening – and making people question its value.
Colon cancer is increasing in younger U.S. adults at a rate of 1.5% annually due to lifestyle, diet, and environmental factors. During the early stages of the COVID-19 pandemic, many preventive screenings were postponed. If patients and providers don’t take colon cancer screening seriously, there is significant risk of an increase in preventable colon cancers and deaths.
Let’s take a closer look at what the NordICC data really mean and why broad assumptions from it can’t be applied automatically to the U.S. population.
Inside the numbers of Nordic ICC
The Northern-European Initiative on Colorectal Cancer (NordICC) trial was a randomized clinical study of almost 85,000 people in Poland, Norway, Sweden, and the Netherlands from 2009 to 2014, with follow-up planned for 15 years.
Of these people, 28,220 people were chosen at random to be invited to get a colonoscopy, just 42% of whom actually completed the exam and some of whom likely were driven to do so because they were experiencing gastrointestinal symptoms.
Researchers followed the entire group of 28,220 people who were invited to participate for 10 years and found that:
- 259 cases of colorectal cancer were diagnosed in people who got the colonoscopy
- 622 cases were found in the not-invited (control) group
When all 85,000 patients’ data were considered, colonoscopy was found to reduce cancer incidence by 18% and had no changes in risk of death. These data were compared to data from four large studies on outcomes of sigmoidoscopy – which just examines the lower part of the colon, not the full colon like in colonoscopy – essentially comparing apples to oranges. In patients with average risk, sigmoidoscopy reduces the risk of developing colon cancer by 22% and dying from it by 26%.
But when data from NordICC were narrowed to just the invited participants who got a colonoscopy, the 10-year risk of colorectal cancer decreased by 31% and the risk of colorectal cancer-related death decreased by 50%.
This important study showed that colonoscopy can significantly improve prevention and outcomes with colon cancer. As the first large, randomized colonoscopy study, the data are crucial to help encourage more patients to get screened – and more providers to continue reminding patients about colonoscopy.
However, there are important considerations when comparing data from a European study to our U.S. population.
Comparing U.S. and European demographics
Age and public health transparency
In the U.S., we recommend adults at average risk of developing colon cancer begin regular colonoscopies or an alternative screening method at age 45. If your first colonoscopy shows no sign of cancer or polyps, it is recommended that most patients can wait 10 years between screenings, which are covered by most insurances.
Celebrities such as Katie Couric, Jimmy Kimmel, and Ryan Reynolds have been outspoken about the benefits of getting a colonoscopy – even going so far as to film their own and share the results with the public.
When actor Chadwick Boseman died of colon cancer in 2020 at age 43, the U.S. public received a grim reminder of how aggressive colon cancer can be. Organizations such as the American Society of Gastrointestinal Endoscopy and efforts such as the Screen to Save: NCI Colorectal Cancer Outreach and Screening Initiative consistently raise awareness about the benefits of screening.
In Europe, screening recommendations are less aggressive and are less publicly emphasized. Patients may have one colonoscopy screening in their lifetime after age 50, and some countries set age restrictions around when the screening can be done.
Upon invitation to the NordICC study, less than half of eligible individuals got their screenings. This disengagement could be part of the reason why Norway and The Netherlands were among the World Cancer Research Fund International’s list of 10 countries with the highest incidents of colon cancer – and top 3 for women’s risk – and why the U.S. is not on these lists.
Ethnic and lifestyle differences
The NordICC study did not factor in race or ethnicity. For instance, more than 60% of the study participants were from Poland, whose population is more than 96% of western Slavic origin.
The U.S. is more ethnically diverse, with the number of people identifying as two or more races increasing 276% since 2010. Black, Native American, and Alaska Native people in the U.S. have higher incidence and mortality due to colon cancer.
Another consideration is the general lifestyles of European and American people. In the U.S., we have a higher rate of obesity, type 2 diabetes, and consumption of red and processed meat – all of which are leading risk factors for colon cancer. There’s a reason processed, high-calorie, low-nutrient eating pattern is called the Western Diet. As such, U.S. patients may be at increased risk of colorectal cancer and may develop it at a younger age.
Comfort and skill in the screening room
A major factor in colonoscopy screening quality is based on the time spent in the exam and the skill of the endoscopist – the person administering the colonoscopy. Performance among endoscopists in the NordICC trial was highly variable, and a significant number did not perform thorough exams by U.S. standards as set by the American Society for Gastrointestinal Endoscopy.

Approximately 17% of the NordICC endoscopists did not reach the benchmark goal of examining 95% of a patient’s colon and 29% fell short of the 25% adenoma detection rate (ADR) – finding precancerous polyps in the expected one-fourth of patients 50 or older. This is significant; a 1% increase in ADR decreases the risk of colorectal cancer being diagnosed within three years of a colonoscopy by 3% and related deaths by 5%.
The differences in these colonoscopy quality benchmarks could be due to European endoscopists performing fewer colonoscopies than U.S. endoscopists. And in the U.S., patients are offered anesthesia during colonoscopies, which is less common in Europe.
Less experienced endoscopists conducting a screening without anesthesia might cause more discomfort and move faster in response to the patient’s pain signals, resulting in a less thorough procedure.
Timing of polyp growth
Another reason colonoscopies are effective is that colon cancer is a slow-growing cancer. In general, it takes precancerous polyps approximately 10 years to develop into cancer. Data in the NordICC trial are being reported at the 10-year mark, which means there are still five years of follow-up remaining.
In the U.S., patients at average risk of colon cancer whose colonoscopies reveal polyps are recommended to get another screening at five years instead of 10 in case cancer develops. But in Europe, many countries offer one-time screenings only, starting at 55 years old instead of 45.
It will be interesting to see the NordICC data at 15 years follow-up – in that time, more patients may develop colon cancer due to newly formed polyps or those that were missed during the one-time screening.
You have options for colorectal cancer screening
Colonoscopy is an often-maligned procedure for two primary reasons.
- “Prep” for the exam requires patients to drink a prescribed fluid that helps clear out their bowels so we can get a good look at the colon tissue. But recent improvements in the drink’s formulation have made it taste better and prep more tolerable.
- It is invasive, although colonoscopy doesn’t require any incisions and is a painless, quick outpatient procedure.

Colon cancer screening methods
Get more details about colonoscopy and other screening methods.
If you are at average or low risk of developing colon cancer – meaning no symptoms and no personal or family history of the disease – you can choose other screening methods for colon cancer. Alternative colon cancer screening options include:
- Stool tests: These tests check for blood or altered DNA in your stool (poop). You can collect a sample at home and send it to the laboratory for analysis. Stool tests are repeated every year or every three years, depending on the type of test.
- Flexible sigmoidoscopy: The doctor uses a thin, flexible tube to check your rectum and the lower third of your colon for polyps or cancer. This test is repeated every five years or every 10 years when combined with a stool test.
- CT colonography (virtual colonoscopy): With this option, we use a computer and CT scans to take pictures of the entire colon. The doctor analyzes the images for signs of cancer, repeating the screening every five years.
If polyps or cancer are detected, you will need a follow-up colonoscopy to get a specific diagnosis and/or remove the polyps to be biopsied.
Over time, the NordICC study is likely to reveal more data and we’ll have to examine it to determine if it is useful and relevant for U.S. patients.
Despite the headlines, the ultimate takeaway from the study should be clear: colonoscopies save lives and prevent colon cancer.
To request an appointment for a colon cancer screening, call 214-645-8300 or request an appointment online.