Why follow-up care is crucial when a newborn fails ABR hearing screening
May 25, 2021

Your baby will receive many tests and treatments in their first days of life, from Apgar scoring to measure their reflexes and eye drops that eliminate germs to their first series of vaccinations.
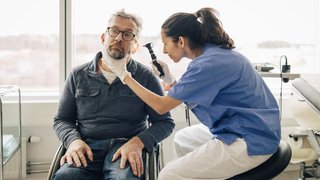
Among the most important of these is the newborn hearing screening. From birth, babies use information from their surroundings to access early language – the foundation for a lifetime of communication.
Babies who are born deaf or hard of hearing need additional support to access language. Knowing early whether a newborn has hearing loss gives families the best chance to improve their hearing and language development.
There are two types of hearing screenings for newborns. Both are painless and work by introducing sound into the baby’s ear and analyzing the ear’s function:
- Otoacoustic emissions (OAE) – the standard that many hospitals use. OAE measures activity from the hair cells in the inner ear that bring sound vibrations to the cochlea, a structure that transforms the vibrations into signals that travel up the brainstem.
- Auditory brainstem response (ABR) – an advanced technology that UT Southwestern and Parkland Health use. ABR assesses more of the auditory pathway, recording neural impulses from the cochlea and all the way through the upper levels of the brainstem.
OAE screening is sufficient for most newborns, but ABR screening reduces the number of vulnerable babies who might get left behind. For example, preemies may have underdeveloped auditory nerves, causing hearing loss. Babies with auditory neuropathy spectrum disorder may have a cochlear response, but sound vibrations don’t make it to their brains.
Using ABR offers parents two layers of confidence in their newborn’s results. A trained technician performs the screening. At some institutions, including Parkland Hospital, if the baby does not pass, they get a second ABR with an audiologist – a doctor who specializes in hearing – before they go home from the hospital.
Angela Shoup, Ph.D., previously Chief of the Division of Communicative and Vestibular Disorders at UT Southwestern Medical Center, and now Executive Director of the Callier Center for Communication Disorders, Professor at UT Dallas and Clinical Professor at UT Southwestern was a champion in developing this advanced process. Learn more below about Dr. Shoup’s 25-year passion for universal newborn hearing screening.
Newborns that do not pass the hospital hearing screening may have acute or chronic hearing loss. These babies need advanced follow-up within two weeks. At that visit, we can determine whether the problem is temporary or chronic – and what the baby needs in order to access early language development.
What causes babies to fail their hearing screening?
Deafness and hearing loss can be caused by genetic abnormalities, birth defects, or maternal infections during pregnancy. In some cases, the baby will immediately show signs of hearing loss, such as not responding to sounds or failing their hearing screening.
Rarely, a baby who can hear and process sound might nonetheless fail their newborn hearing screening. Some of these include babies who:
- Stayed in the NICU: Babies go to the neonatal intensive care unit (NICU) for high-risk health issues, some of which can damage hearing. For example, serious breathing problems can decrease oxygen to the brain, resulting in inner ear or auditory nerve damage. Maternal health complications such as diabetes or substance use disorder can also negatively impact hearing.
- Had fluid in their ears: Some newborns get fluid in their middle or inner ears during the birth process, and it can take a few days for the fluid to clear. Approximately 10 percent of babies with fluid in their ears may develop lasting hearing loss that requires treatment, according to the American Academy of Otolaryngology – Head and Neck Surgery Foundation [PDF].
- Had jaundice: Jaundice is a temporary condition that causes approximately 60 percent of newborns to temporarily have yellowed skin and eyes. The baby’s liver must adapt to filtering out the chemical bilirubin – which is handled by the mother’s liver during pregnancy. Short-term elevations of bilirubin levels, as well as severe and untreated jaundice, can cause hearing loss.
- Had a CMV infection: Congenital cytomegalovirus (CMV) is a viral infection that can cause severe disease if a baby is infected before birth. In the U.S., 0.5-0.7 percent of babies are born with CMV, and approximately 90 percent of those have no symptoms at birth. However, 10-15 percent of asymptomatic babies develop hearing loss over time. Visit the National CMV Foundation to learn more.
- Aspirated meconium: Occasionally, a baby swallows their own feces (poop) during birth. With quick treatment, breathing complications generally resolve quickly. However, some antibiotics used to treat meconium-related infections, such as gentamicin, can damage the sense organ of hearing.
If your baby experienced these issues and passed their newborn hearing screening, they still will likely need follow-up screenings throughout childhood. Hearing loss can develop over time, and your baby may need close monitoring and screening for hearing loss through young adulthood.
If the baby did not pass the newborn hearing screening, it’s important that the baby receive an advanced follow-up screening within 10-12 days for the best chance at receiving early intervention and unlocking their early language development.
The advanced follow-up visit is crucial
Because UT Southwestern uses highly sensitive ABR screening for all newborns, many babies who are referred for advanced follow-up screening have some level of hearing impairment. Keeping the advanced follow-up visit is crucial to give your newborn a healthy start in language development.
We understand that attending another appointment with a newborn takes extra work. But there are serious health consequences for infants who do not get the advanced care they need, including delayed speech, social isolation, and lifelong communication problems at school, at work, and in interpersonal relationships.
What to expect at the advanced follow-up visit
Your baby will get an outpatient ABR screening.
- If the baby passes this advanced screening, we will give you important information about hearing and speech development milestones. We’ll also refer you for regular follow-up screening if your baby has a risk factor for delayed onset of hearing loss, which can develop later in childhood.
- If the baby does not pass, we will refer you to Children’s Health for a diagnostic evaluation by a pediatric audiologist and otolaryngologist (ear, nose, and throat doctor). At the appointment, the audiologist will complete a diagnostic ABR evaluation that helps us determine at which volumes, pitches, and frequencies the baby can receive sound.
We will guide and support you through every step of evaluation, diagnosis, and treatment. With early diagnosis, there are many options to improve how your baby accesses sound, develops language, and learns to communicate.
Treatment options for babies with hearing loss
With proper support, deaf or hard of hearing babies can grasp language and develop on track with their peers. Our goal is to maximize any hearing they have and supplement language development with multichannel support.
Depending on the type and severity of hearing loss, babies through young adults can benefit from:
- Getting cochlear implants – surgically implanted devices that stimulate the auditory nerves to improve sound transmission
- Using amplification devices or hearing aids
- Learning American Sign Language (ASL)
- Some types of ear surgeries, if the part of the ear behind the eardrum is not fully developed or the bones in that part of the ear have congenital abnormalities
- Accessing accommodations at school, such as sitting closer to the teacher or getting written notes
- Connecting with other deaf or hard of hearing people, socially or in support groups

Children’s Health Family-Focused Center for Deaf and Hard of Hearing Children can connect you with community resources to keep your child’s development on track, as well as offer emotional support for children and parents.
Universal hearing screening and early intervention for infants who are deaf or hard of hearing can generate positive impacts on society as a whole. Citizens who learn to communicate – with speech, ASL, or both – can enjoy interacting with their peers and contribute more productively to society than if their hearing loss was left untreated.
Early hearing loss intervention offers parents a chance to bond with their baby and help them thrive. And pediatric intervention services can spare children from the stress and depression that can arise from potentially isolating disabilities such as hearing loss.
When it comes to hearing difficulties, time is of the essence. The quicker we identify and quantify your child’s hearing abilities, the sooner we can help get them the advanced care they need.
Innovation spotlight: How UT Southwestern faculty, affiliates led the Texas journey to universal newborn hearing screening

Angela Shoup, Ph.D., is a champion for newborn hearing screening. She was Chief of the Division of Communicative and Vestibular Disorders at UT Southwestern Medical Center and is currently the Executive Director of the Callier Center for Communication Disorders at UT Dallas, a professor at UT Dallas and a clinical professor in the department of Otolaryngology at UT Southwestern.
Evolution of Hearing Screening in Texas
- 1960s: National advocates begin working toward universal newborn hearing screening.
- 1970s: The Joint Committee on Infant Hearing recommends developing a high-risk registry for screening, inclusive of factors we still use today in determining a child’s chances for delayed onset or progressive hearing loss, such as infections or premature birth.
- 1986: Supported by the National Council of Jewish Women, Parkland begins newborn hearing screenings for all babies at high risk for hearing loss, as well as all babies in special care nurseries, regardless of known risk factors.
- 1993: The National Institutes of Health recommends that all infants need an ABR or OAE hearing screening by three months of age, and that appropriate follow-up should be established for babies who do not pass.
- 1996: Dr. Shoup joins the UT Southwestern faculty with a passion for newborn hearing and early language access.
- 1997: Dr. Shoup and Kristine Owen, Au.D., a UT Southwestern audiologist, work with a multidisciplinary team including representatives from the Parkland nursery nurse and nurse practitioner leadership, physician leadership, and Women and Children’s Health leadership to plan for universal newborn hearing screening at Parkland. Pablo J. Sanchez, M.D., an infectious disease neonatologist, advocated for the addition of hearing-targeted congenital cytomegalovirus screening to the protocol.
- 1999: The team earns a grant from the Hoblitzelle Foundation to equip Parkland with the necessary equipment to launch universal newborn hearing screening – one year before it is required by the passing of Texas House Bill 714.
- 2000-present: Dr. Shoup works with organizations involving multiple stakeholders, including physicians, audiologists, early intervention specialists, educators, speech-language pathologists, and others, to ensure providers and families understand the importance of newborn hearing screening for lifelong health and communication.
- 2008: Drs. Stehel, Shoup, Sanchez, and Owen, et al., publish a study in Pediatrics associating the discovery of CMV infections in infants based on abnormal newborn hearing screening results.
- 2016: Dr. Shoup receives the UT Dallas Distinguished Alumni Award.
- 2018 & 2019: Dr. Shoup is named a D Magazine Best Doctor and inducted into the National Academies of Practice Audiology Academy as a Distinguished Scholar and Fellow.
- 2020: Parkland Health maintains a strong follow-up program, with nearly 100% of infants that do not pass hearing screening returning for follow-up visits.
- 2021: Dr. Shoup currently serves as President of the American Academy of Audiology and Vice Chair of the National Academies of Practice Audiology Academy.
Schedule a visit with a pediatric hearing expert. Call 214-645-8300 or request an appointment online.