Caring for High-Risk Babies
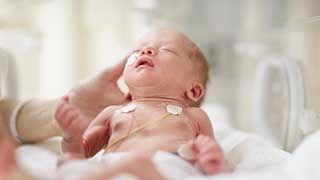
Babies considered high-risk have a greater chance of complications due to conditions that occur during fetal development, pregnancy conditions of the mother, or problems that might occur during labor and birth. Some complications are unexpected and can occur without warning. Other times, there are certain risk factors that make problems more likely.
Fortunately, advances in technology have helped improve the care of sick newborns. Under the care of UT Southwestern’s specialized physicians and other health care providers, at-risk babies today have much greater chances for surviving and getting better than ever before.
Care at Parkland Memorial Hospital
UT Southwestern’s neonatologists provide care for both healthy and sick babies at Parkland Memorial Hospital.
- Neonatal Intensive Care Unit: Our 96-bed Level III NICU averages about 1,400 admissions a year. Our team of physicians, nurses, and support staff is highly experienced in caring for a wide array of neonatal disorders. This teamwork has resulted in one of the lowest mortality rates in the country.
- Newborn Nursery: With more than 12,000 deliveries a year, the newborn nursery at Parkland is one of the busiest in the country. Under the supervision of UT Southwestern faculty, pediatric residents and pediatric nurse practitioners provide comprehensive care for both term and near-term infants from birth through discharge.
- Labor and Delivery: We provide a unique and highly trained neonatal resuscitation team that attends more than 300 high-risk deliveries each month. We have the capability to deliver cutting-edge delivery room care in even the most complex cases, including EXIT (Ex Utero Intrapartum Treatment) procedures.
Care at Children’s Medical Center Dallas
Babies with special metabolic, cardiac, or surgical conditions can be transferred from other hospitals to the Children's Medical Center NICU, a Level IV NICU that is also supervised by UT Southwestern faculty. This state-of-the-art, 47-bed facility is the premier referral unit in North Texas. Our physicians work with well-trained and experienced nurses, nurse practitioners, and other health care professionals to provide the best care, with the patient's well-being as their first priority.
A wide range of additional neonatal intensive care services are available that span the spectrum of patients from fetus to age 5, including:
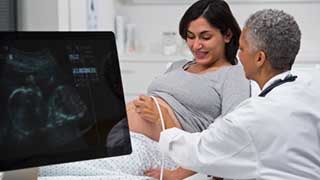
- Fetal Evaluation and Treatment Alliance (FETAL): FETAL is the only program in North Texas offering specialized care for pregnant women diagnosed with a fetal anomaly. Patients, families, and their referring providers participate in prenatal conferences with a highly specialized multidisciplinary team that brings the expertise of UT Southwestern’s subspecialists to the baby at risk. A personalized approach addresses each in utero diagnosis to determine the best strategy for pregnancy, delivery, and continuity of care after birth.
- TeleNICU: The state’s first dedicated neonatal telemedicine service and one of the most sophisticated systems of its kind in the nation, TeleNICU links specially trained, board-certified UT Southwestern neonatologists at Children’s Medical Center to physicians at other hospitals’ NICUs to consult and assist in the management of the sickest and most fragile infants.
- Low Birth Weight Clinic (Thrive Program): Thrive provides comprehensive medical and psychosocial follow-up treatment for NICU graduates through intensive intervention, education, social services, and developmental testing for high-risk infants from birth to age 5.
We also offer:
- Multidisciplinary disease-specific teams, including the Bronchopulmonary Dysplasia and Pulmonary Artery Hypertension Team, the Intestinal Failure Team, and the Congenital Diaphragmatic Hernia Team
- Support services provided through a family support team, including a psychologist, social worker, case manager, child life specialist, and chaplain
- State-of-the-art ventilatory support, including high-frequency ventilation
- High-level subspecialty consultation
- Advanced radiology and other technology with neonatal expertise
- Extracorporeal membrane oxygenation (ECMO)
- Cardiothoracic surgery and anesthesia program
- Fetal and postnatal echocardiography
- Lactation specialists
- On-site neonatal pharmacy services
- Pediatric ostomy specialists
- Video EEG for evaluation of seizures
Care at William P. Clements Jr. University Hospital
At William P. Clements Jr. University Hospital, we provide the highest level of neonatal care in a warm and inviting environment that helps parents to connect with their baby.
- Level III Neonatal Intensive Care Unit: Clements University Hospital features 30 NICU rooms, giving each baby his or her own room, in a space sized to easily accommodate both hospital staff and parents. State-of-the-art neonatal care including mechanical ventilation (both conventional and high frequency), inhaled nitric oxide therapy, and outstanding nursing care are provided to fragile infants. Parents can sleep in the room overnight with their newborns – enabling parents to focus on their infant and build bonds that will help the baby grow stronger. Research shows that more parental involvement helps babies with weight gain, breastfeeding, and earlier release from the hospital.
- Newborn Nursery: Our labor, delivery, and recovery rooms combine modern technology with a warm, homelike environment to provide a safe and comfortable experience for mothers and families. Our highly experienced newborn physicians provide expert care for the newborn infant. We also have lactation consultants to provide breastfeeding assistance.