The Peter O’Donnell Jr. Brain Institute brings together transformative research and patient-centered care to improve the lives of patients today and those of generations to come.
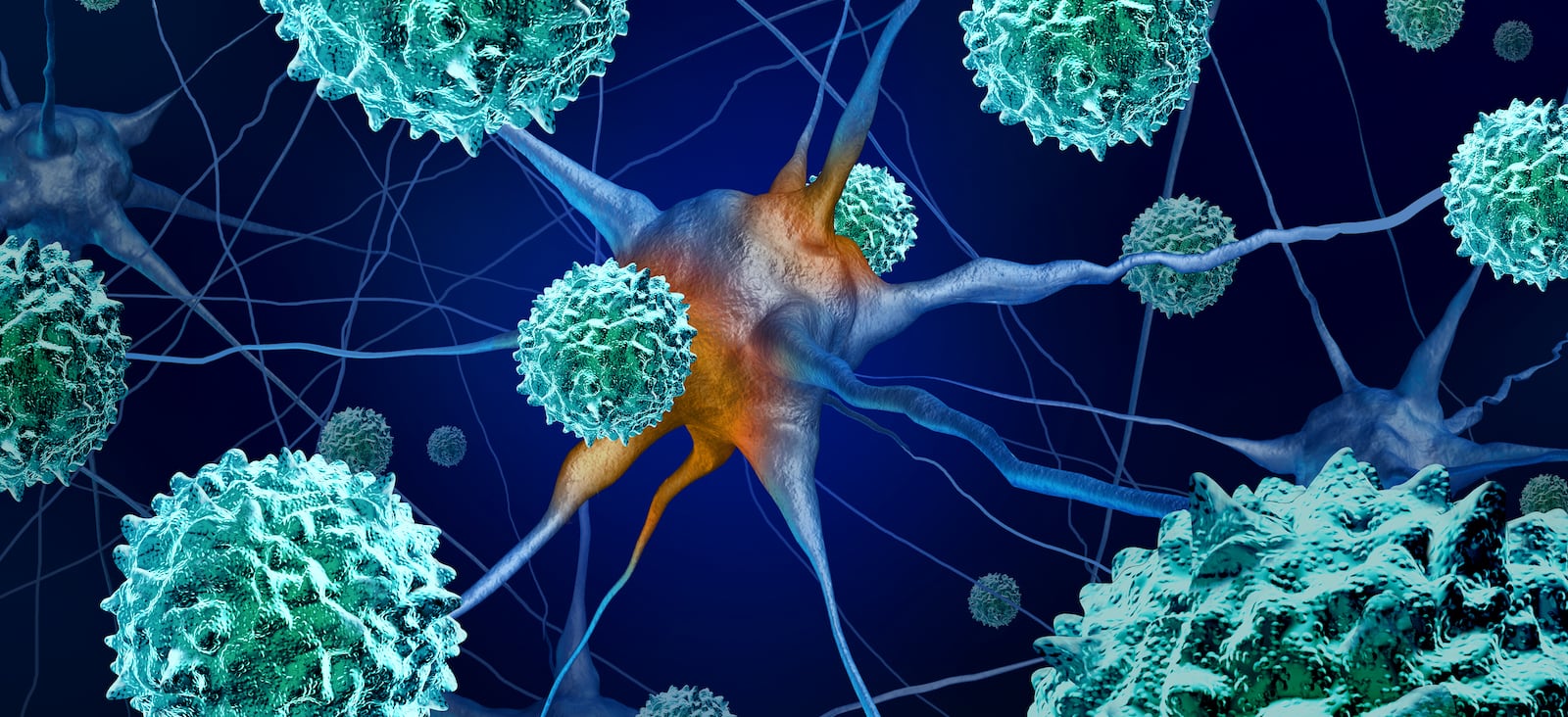
Enteroviruses are a group of viruses that usually causes flu-like symptoms or gastrointestinal illness. Most people don’t get sick, or if they do, they experience mild symptoms such as fever, body aches, cough, and nasal congestion. In rare cases, enteroviruses can cause severe, life-threatening illnesses, usually in infants, young children, and people with weakened immune systems.
Diseases and symptoms caused by enteroviruses include:
- Hand-foot-and-mouth disease
- Heart infections such as myocarditis and pericarditis
- Hemorrhagic conjunctivitis, a more severe form of pinkeye
- Nervous system (brain and spinal cord) infections such as encephalitis and meningitis
- Respiratory infections such as colds, pneumonia, and sinus infections