The Peter O’Donnell Jr. Brain Institute brings together transformative research and patient-centered care to improve the lives of patients today and those of generations to come.
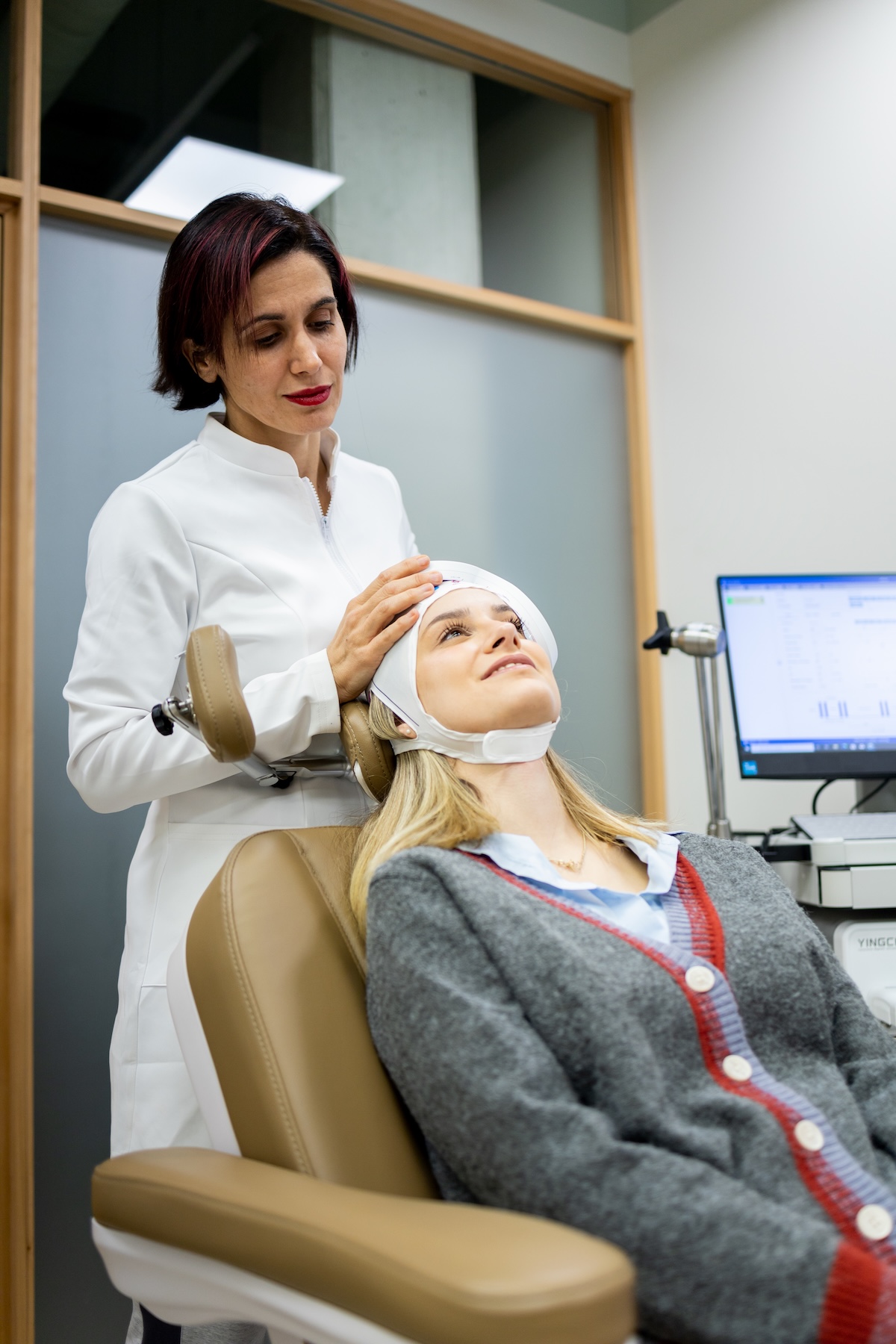
Interventional Psychiatry
New Patient Appointment or 214-645-8300
MedBlog
Results: 2 Locations
Multispecialty Psychiatry Clinic
at UT Southwestern at Empire Plaza 1 1430 Empire Central Drive, 1st FloorDallas, Texas 75247 214-645-8500 Directions to Multispecialty Psychiatry Clinic at UT Southwestern at Empire Plaza 1, Dallas Parking Info for Multispecialty Psychiatry Clinic