Expert Care for Coronary Artery Diseases
The heart supplies the body – and itself – with blood through a network of vessels called coronary arteries. The coronary arteries can narrow and become blocked from a buildup of cholesterol and fat called plaque (atherosclerosis).
When that happens, the heart muscle might not get enough blood to continue working properly. This condition is coronary artery disease (CAD).
If a portion of the plaque buildup in the coronary arteries ruptures, a blood clot forms that can block the artery entirely, starving the heart of oxygen. This situation leads to the emergency known as myocardial infarction (heart attack). Even when a heart attack is not fatal, it can seriously damage heart muscle.
Over time, coronary artery disease also can weaken the heart and lead to heart rhythm abnormalities (cardiac arrhythmias) or heart failure.
The UT Southwestern Preventive Cardiology team helps patients understand their risk for coronary artery disease through detailed assessments and tests, as well as an evaluation of hereditary risk factors and other conditions that could impact their heart health. Our team then works with patients to reduce risk through interventions such as lifestyle modifications and medications to lower blood pressure and reduce plaque within coronary arteries.
For patients who have more advanced disease requiring more aggressive treatment, our Interventional Cardiology team provides expertise in evaluating and clearing clogged arteries with catheter-based techniques such as:
- Coronary angiogram to visualize blood vessel blockages
- Angioplasty to open up clogged coronary arteries to restore blood flow
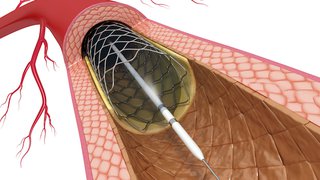
- Placement of a stent – a small, cage-like structure – to hold a cleared artery open
When severe coronary artery disease affects multiple blood vessels, open-heart bypass surgery, known as coronary artery bypass graft, or CABG, might be the most appropriate treatment. UT Southwestern’s Department of Cardiovascular and Thoracic Surgery is one of the nation’s leading programs, with fellowship-trained surgeons performing more than 600 open-heart procedures each year.
Whatever a patient’s degree of coronary artery disease or risk for developing it, our multidisciplinary team of cardiologists and cardiothoracic surgeons will discuss options and tailor a treatment plan to the patient’s condition, goals, and lifestyle.
What Is Coronary Artery Disease?
The heart’s intricate system of chambers, valves, and blood vessels recycles, replenishes, and recirculates about 2,000 gallons of blood per day. The heart obtains its own blood supply from two arteries that originate just above the aortic valve: the left main coronary artery and the right coronary artery. These arteries branch off into smaller arteries that supply the heart’s chambers and tissues with nutrient-rich blood.
As people age, fat can build up in the walls of the coronary arteries. Calcium, protein, and other materials moving through the blood vessels stick to the fat, forming a material called plaque. This buildup of plaque – a condition called atherosclerosis – occurs more rapidly in some people than others.
As the plaque layer thickens, blood flow to the heart can be reduced, damaging the heart muscle. If coronary artery disease goes undiagnosed and untreated for an extended period of time, the heart will weaken and pump blood less efficiently. This condition is known as heart failure. Should the flow of blood become completely blocked in one or more arteries, a heart attack can result, sometimes with deadly consequences.
Though treatment of heart attacks has improved dramatically in recent decades, coronary artery disease remains the leading cause of death for both men and women in the U.S.