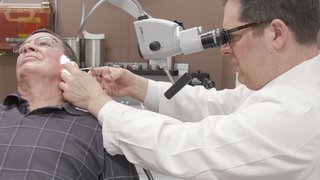
Unique Challenges Solved by Expert Surgeons
Skull base disorders involve the bony shelf that separates the brain from the eyes, nasal cavities, ear canals, and upper neck. Major nerves, blood vessels, and other structures pass through this area, making treatment of skull base conditions complex.
Skull base disorders present unique challenges to surgeons. Combining a multidisciplinary approach with the latest technology and most advanced techniques, our physicians have extensive experience in the latest minimally invasive techniques that have revolutionized the field of skull base surgery.
Many formerly inoperable tumors can now be reached using a very small telescope through the patient’s nasal passages, eliminating the need for facial incisions. Surgery can be performed with minimal brain manipulation, thus minimizing complications and preserving normal neurologic and facial function.
In addition, evaluation and treatments are coordinated with specialists at the UT Southwestern Harold C. Simmons Comprehensive Cancer Center, so patients can see all the physicians involved in their care in one setting. All patients with skull base tumors are seen promptly. Same-day and next-day appointments are often available.
About Skull Base Disorders
The UT Southwestern team is experienced in the diagnosis and management of a wide range of skull base disorders, such as:
Treating Skull Base Disorders
To properly treat skull base disorders, UT Southwestern uses a multidisciplinary team of physicians from a range of specialties, such as neurosurgery, neuro-ophthalmology, neurologic oncology, radiation oncology, interventional radiology, otorhinolaryngology-head and neck surgery, and pathology. These specialists develop an individualized treatment plan for each patient and carefully coordinate care.
The evaluating physician gathers information about the patient’s current disease status, any chemotherapy medications taken, and any previous treatments that were performed.
Our physicians can then make precise preoperative plans using high-definition magnetic resonance imaging (MRI) and computed tomography (CT) scanners. We also use image-guidance technology to achieve precise surgical goals. In many instances, tumor removal can be achieved with minimal disturbance to the surrounding normal structures.
In addition, our program offers:
- Removal of skull base tumors in a combined procedure performed by neurosurgeons, rhinologists, neuro-otologists, and head and neck surgeons (craniofacial resection)
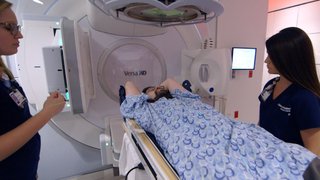
- State-of-the-art radiation therapy technology, such as:
- CyberKnife (stereotactic body radiation therapy)
- Gamma Knife
- Image-guided radiation therapy
- Intensity-modulated radiation therapy
- Additional services such as audiology, vestibular testing, and facial nerve rehabilitation